What Does a Spravato Session Actually Feel Like?

If you're considering Spravato and you've done any research, you've probably found a lot of clinical information about how it works in the brain. What's harder to find is a plain-language answer to the more immediate question:
What is it actually like to sit through a session?
Before You Arrive
Spravato is FDA-approved for treatment-resistant depression, meaning it's typically prescribed when at least two antidepressants haven't produced adequate relief. Before your first session, you'll have a consultation and medical screening to confirm you're a suitable candidate. There are some contraindications, so this step matters.
A few practical things to sort before each appointment:
You can't drive yourself home. Spravato can temporarily affect your perception and alertness, so you're required to have someone pick you up - or arrange another way home. This applies after every session, not just the first one.
Don't eat a heavy meal beforehand. Nausea is a possible side effect, and arriving on an empty or light stomach helps. Your clinical team will give you specific guidance on this.
Plan your day around it. Each appointment runs for at least two hours - the session itself plus the mandatory monitoring period afterwards. Don't schedule anything demanding immediately after.
During the Session
The medication itself
Spravato is a nasal spray. You self-administer it under the supervision of a clinician; they're present throughout, but you operate the device yourself. The active ingredient, esketamine, is absorbed through the nasal lining and gets to work relatively quickly.
Dosage is either 56mg or 84mg, determined by your physician based on your treatment plan.
What you'll feel
Most patients experience some degree of dissociation, a feeling of being slightly detached from their surroundings, or a sense that things feel a little unreal. This is a known, expected effect of esketamine. It isn't the same as losing consciousness. You're aware of where you are. It's more like a shift in how present or grounded you feel.
Other common experiences during a session include:
- Dizziness or light-headedness
- Distorted perception, sounds or visuals may feel slightly different
- Drowsiness or a heavy, relaxed feeling
- Nausea in some cases
- A temporary increase in blood pressure (which is why monitoring happens)
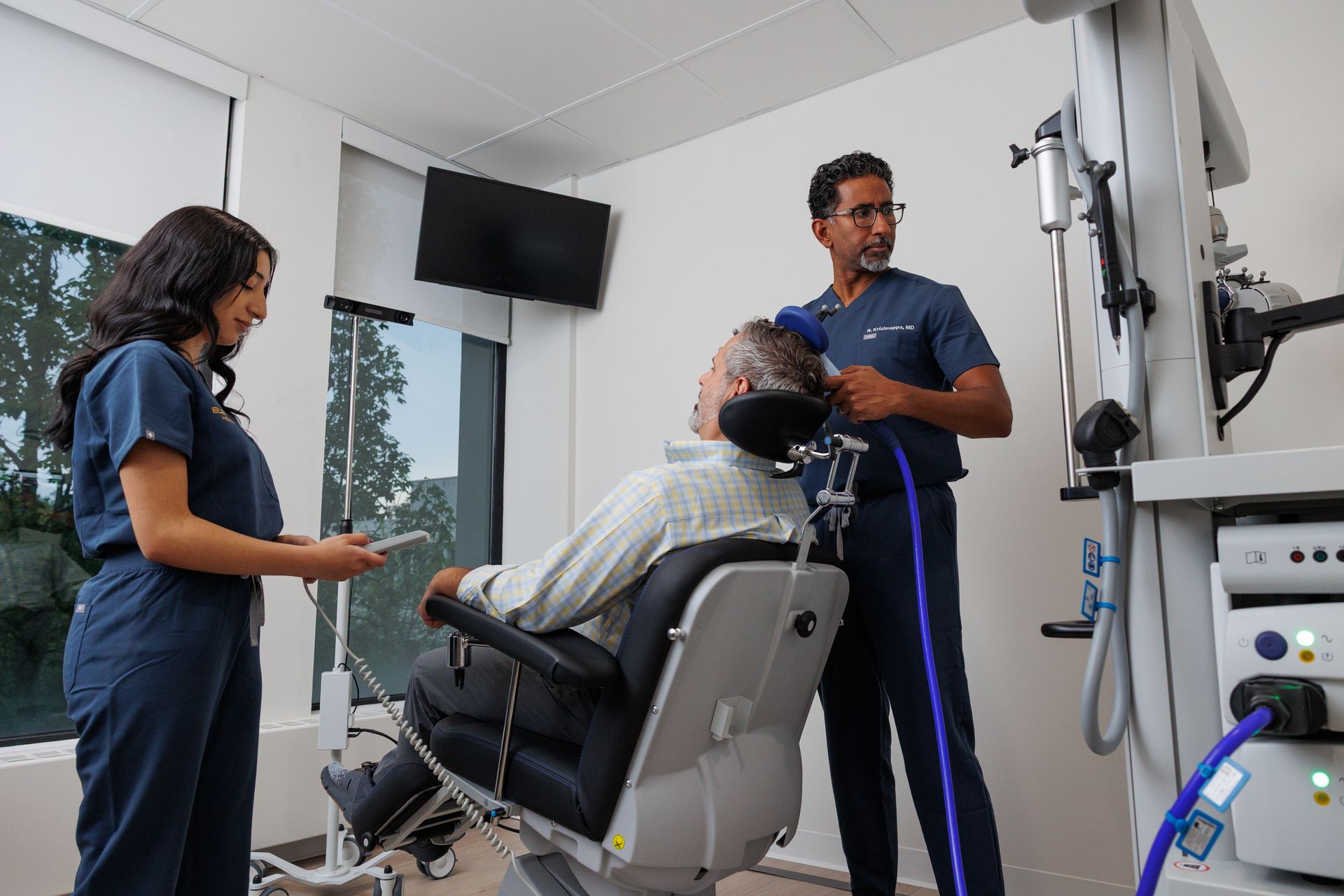
The environment at Elevium
Sessions take place in a dedicated treatment room. You'll be in a zero-gravity reclining chair, designed to be comfortable for the duration. The clinic plays music selected for its calming effect. The goal is to make the environment as settled and low-stimulation as possible while the medication does its work.
A clinician is available throughout. You're not left alone.
The Two-Hour Monitoring Period
After you administer Spravato, you stay at the clinic for at least two hours. This is a regulatory requirement, not just a precaution. Elevium Health is a REMS-certified Spravato treatment centre, which means strict protocols around post-session monitoring are part of the programme.
During this time, your blood pressure is checked, and your clinical team monitors how you're feeling. Most patients spend this period resting, some doze off, some sit quietly, and some feel well enough to read or listen to music.
You won't be cleared to leave until your clinician is satisfied that the acute effects have sufficiently resolved.
After You Leave
Once you're home, the main thing to know is that the day is effectively done for anything requiring sharp concentration. No driving for the rest of the day. Most patients feel tired afterwards and find that resting or sleeping is the natural response.
The dissociative effects are temporary. They don't carry over into the following day for most people.
What does carry forward, often within hours of the first session, and increasingly over subsequent sessions, is the therapeutic effect. Improved mood. Reduced suicidal ideation for those experiencing it. A sense that something has shifted. It doesn't happen for every patient at the same pace. Still, Spravato's capacity for rapid relief is one of the reasons it's used for treatment-resistant cases where waiting weeks for an antidepressant to kick in isn't a viable option.
How Often Do Sessions Happen?
Spravato follows a phased schedule:
- Induction (weeks 1–4): Two sessions per week
- Optimisation (weeks 5–8): Once a week, adjusted based on your response
- Maintenance (ongoing): Every one to two weeks, as needed
So in the early weeks, you'll be coming in twice a week and giving roughly half a day to each appointment. It's worth factoring that into your planning before you start.
A Realistic Note on What to Expect
Spravato works for a lot of people, particularly those who haven't responded to other treatments. But the experience of a session isn't always comfortable. The dissociation can feel disorienting, especially at first. Some patients find the monitoring period long. Nausea is a real possibility.
The reason people go through it is that, for treatment-resistant depression, the alternative is continuing not to get better. For many patients, the discomfort of a session is a fair trade for the relief that follows.
If you want to know whether Spravato is likely to be a good fit for you specifically, that conversation starts with a consultation.
Will I lose consciousness during a session?
No. Spravato can make you feel dissociated or drowsy, but you remain aware of your surroundings throughout. It's not an anaesthetic experience.
Can I go back to work afterwards?
Not on the same day. The effects on alertness and perception mean you shouldn't drive or do anything requiring sharp concentration for the rest of the day after each session.
How quickly does it start working?
Some patients notice a shift in mood within hours of their first session. For others, the effects build over the first few weeks. It varies,; your clinical team will monitor your response and adjust accordingly.
Is it covered by insurance?
Spravato is covered by many major insurers for treatment-resistant depression. Coverage varies by plan. Elevium's team can help you verify your benefits before you begin.
Share Article