From OCD Symptoms to Daily Relief - One Patient’s TMS Journey (Joe)
“I went in with OCD symptoms, and after treatment I’m feeling much better… the staff was wonderful - I highly recommend the crew at Elevium.”
Joe K., former patient
When someone with obsessive-compulsive disorder (OCD) finds a treatment that improves day-to-day life, their story becomes a helpful roadmap for others. Joe K.’s short, honest testimonial does exactly that: it shows what clinical progress looks like and reminds us that compassionate care matters just as much as effective treatment.
Below, we use Joe’s experience as a human anchor to explain how Transcranial Magnetic Stimulation (TMS) is used for OCD, what a typical program involves, and practical advice for people and families thinking about this option.
Joe’s Experience in His Own Words
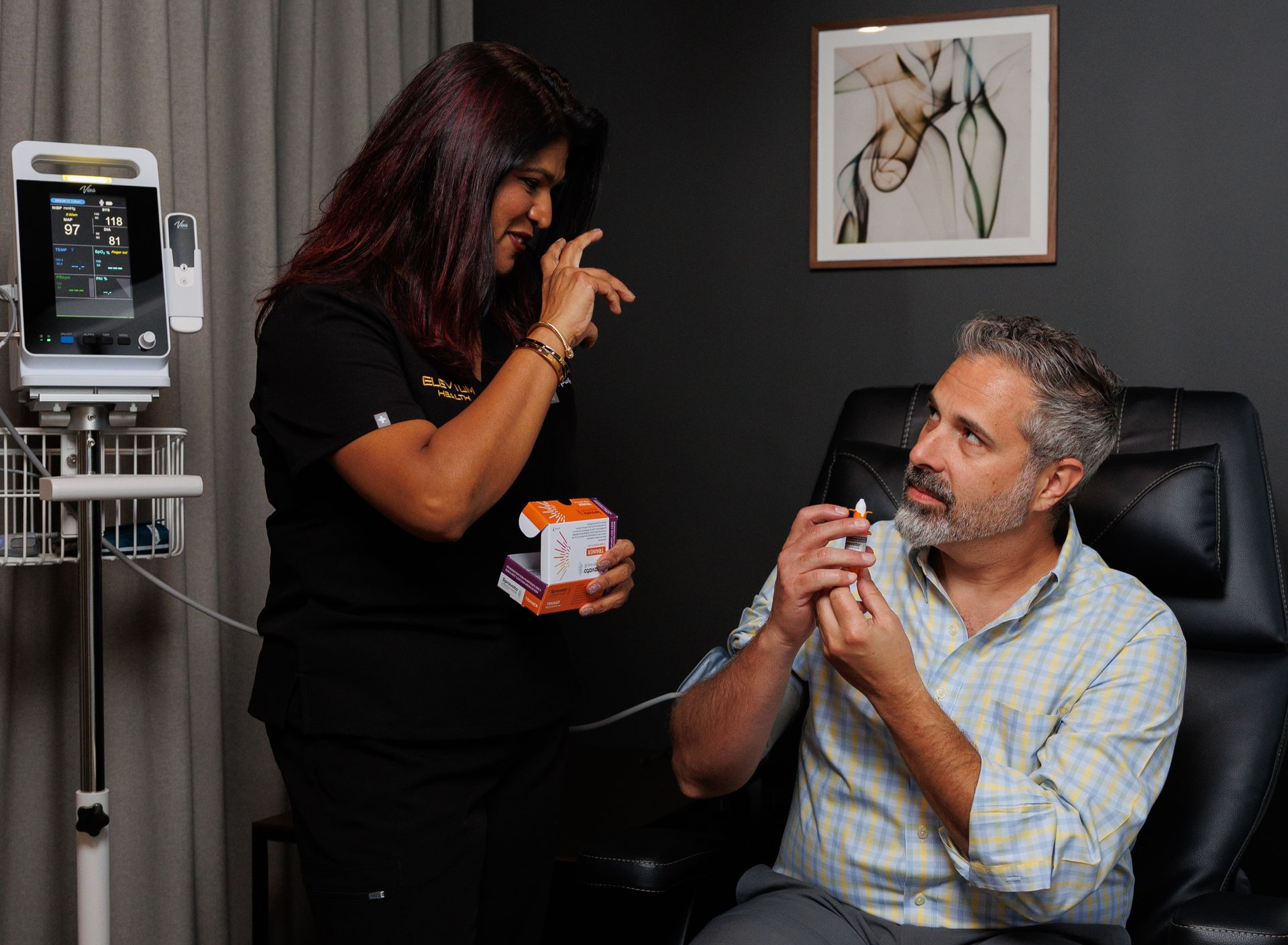
Joe came to Elevium seeking relief from OCD symptoms. His report is straightforward: after a course of TMS, he felt meaningful improvement, and he was impressed with the clinic team’s care and professionalism. That combination -measurable symptom change plus strong clinical support — is what many patients say makes treatment successful.
(Source: Joe’s testimonial.)
A clinician’s View: Why TMS Can Help OCD
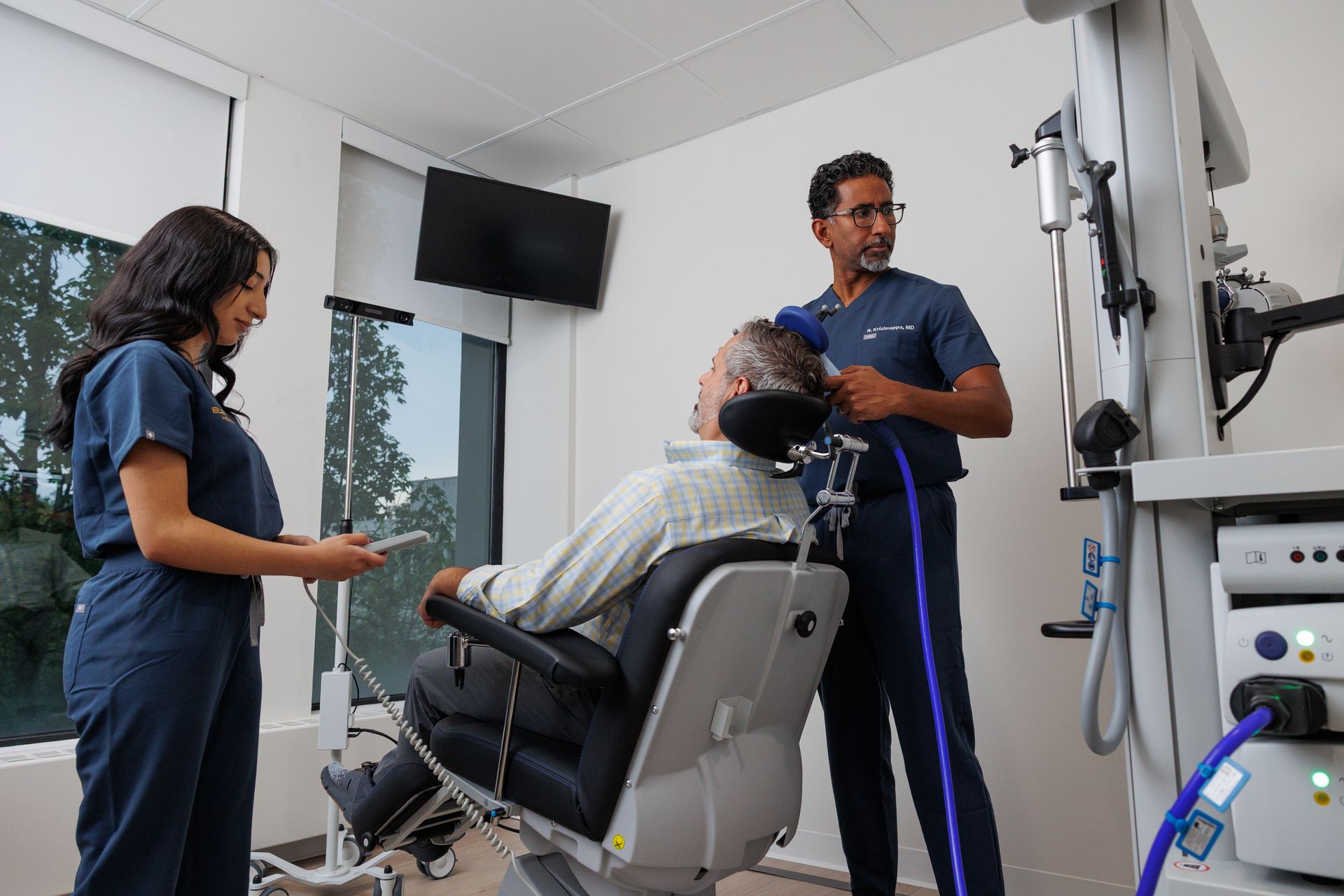
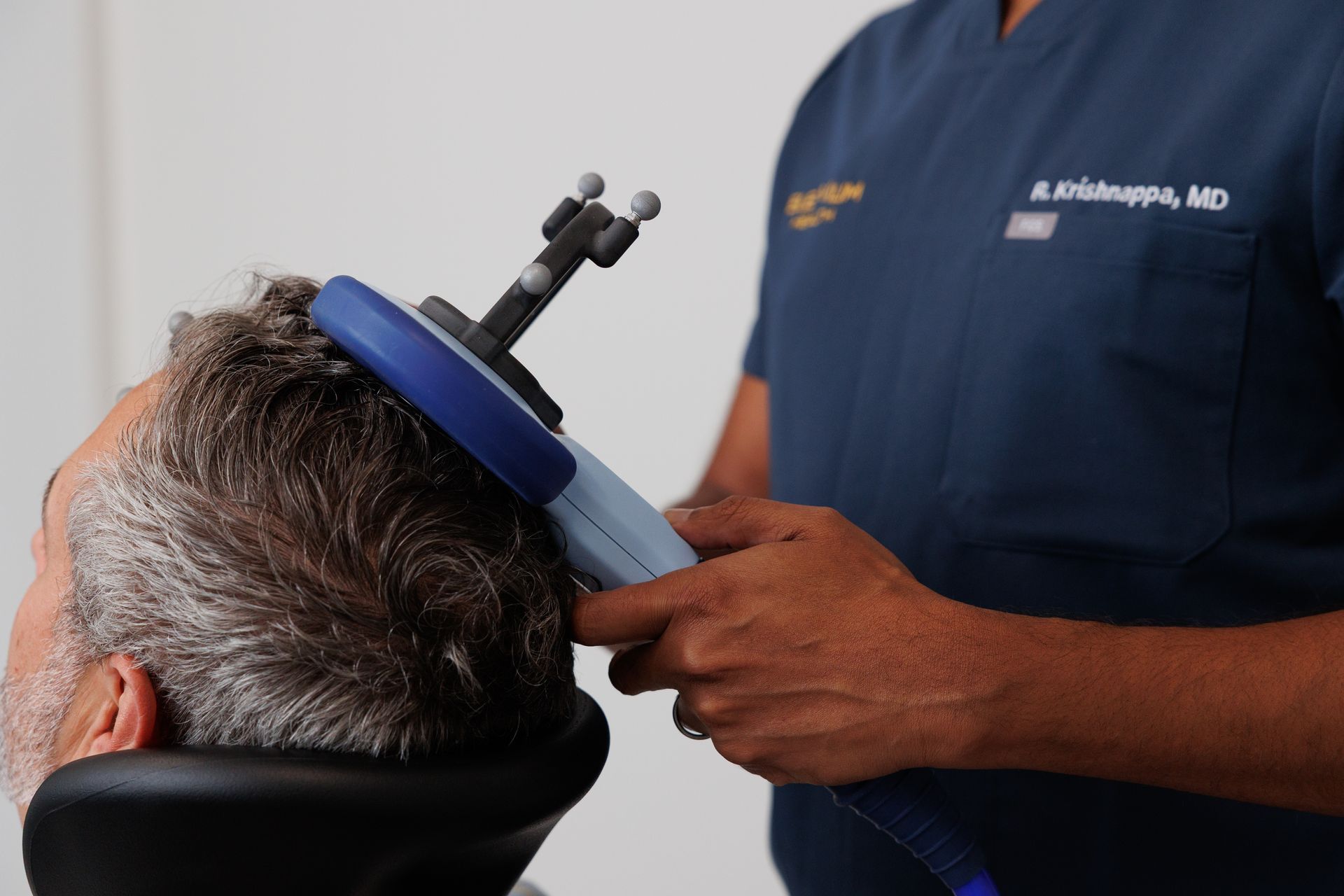
TMS is a non-invasive therapy that uses focused magnetic pulses to influence brain circuits tied to mood, intrusive thoughts, and compulsive behaviors. While TMS is widely used for depression, specialized protocols target cortical and cortico-striatal pathways involved in OCD. Clinical teams deliver tailored stimulation patterns to reduce the intensity and frequency of intrusive thoughts and compulsions. Elevium’s approach follows the evidence-based protocols clinicians use for OCD and integrates careful monitoring throughout treatment.
What a Typical TMS Program for OCD Looks Like
Although protocols differ between centers, an OCD-focused TMS program commonly includes:
- Initial evaluation. A comprehensive clinical assessment (psychiatric history, medical screening, medication review) to confirm candidacy and rule out safety concerns.
- Daily sessions. Most programs provide daily outpatient sessions five days per week over several weeks; each session usually takes 20–40 minutes.
- Ongoing monitoring. Clinicians track symptom changes and side effects and adjust the protocol as needed.
- Integrated aftercare. Outcomes improve when TMS is combined with psychotherapy (CBT) or medication management, and some patients later receive booster sessions to maintain gains.
Joe’s story emphasizes the team element - staff who support scheduling, answer questions, and help patients manage the logistics of daily treatment. That practical support reduces drop-out and improves real-world outcomes.
What the Evidence Says
Research and clinical experience show that when OCD-specific TMS targets are used, a meaningful percentage of patients - particularly those who have not responded fully to medication and therapy — experience reductions in intrusive thoughts and compulsions. Results vary by individual, but
combining TMS with evidence-based psychotherapy produces greater, longer-lasting improvements in many cases.
Practical Advice for Patients & Families
- Plan the logistics. Daily visits require scheduling time for travel, work, or school. Ask the clinic how they help out-of-town patients or offer flexible appointment windows.
- Bring a support person if needed. Having a friend or family member help with scheduling and transportation can ease the burden of daily visits.
- Pair TMS with therapy. Many patients do best when TMS is combined with CBT or another structured psychotherapy.
- Expect a process. Improvement is usually gradual across the treatment course; clinicians will track progress and recommend follow-up or boosters if needed.
Next Steps at Elevium
If Joe’s experience resonates, the first step is a clinical consult to determine candidacy and build a personalized plan. During that consult, you’ll review medical history, discuss expected outcomes, and create a schedule that fits your life.
Elevium’s team can also advise on travel, payment options, and how TMS fits with ongoing therapy.
Is TMS safe for OCD?
Yes - TMS is non-invasive and generally well tolerated. Clinicians screen for seizure risk and other contraindications
How long do results last?
Many patients see benefits that last months or longer; some opt for occasional booster sessions. Long-term outcomes improve when TMS is combined with psychotherapy.
Will I need time off?
Most patients resume normal activities after sessions, but daily scheduling depends on travel and clinic hours. Discuss logistics with the clinic.
Share Article