TMS for Anxiety: Evidence, Protocols, and Patient Profiles

Quick answer
TMS - a non-invasive brain stimulation therapy - is an emerging, evidence-based option for some anxiety disorders, especially when anxiety appears with depression or is resistant to standard treatments. Protocols vary (standard rTMS, iTBS, and device-specific approaches), and candidacy depends on diagnosis, prior treatment history, and medical safety screening. Elevium offers TMS as part of an integrated plan that pairs neuromodulation with psychotherapy and medication management when appropriate.
What the evidence says (short)
Research on TMS for anxiety disorders is growing. Clinical trials and real-world studies show promising improvements for generalized anxiety disorder (GAD), panic disorder, and anxiety that co-occurs with depression. Outcomes vary by diagnosis, treatment history, and the specific TMS protocol used. Unlike the large evidence base for TMS in major depressive disorder, anxiety research is more heterogeneous - but many clinics, including Elevium, consider TMS a reasonable next step when therapy and medications are insufficient. Clinicians track outcomes with validated scales such as the GAD-7 and PHQ-9 to measure change.
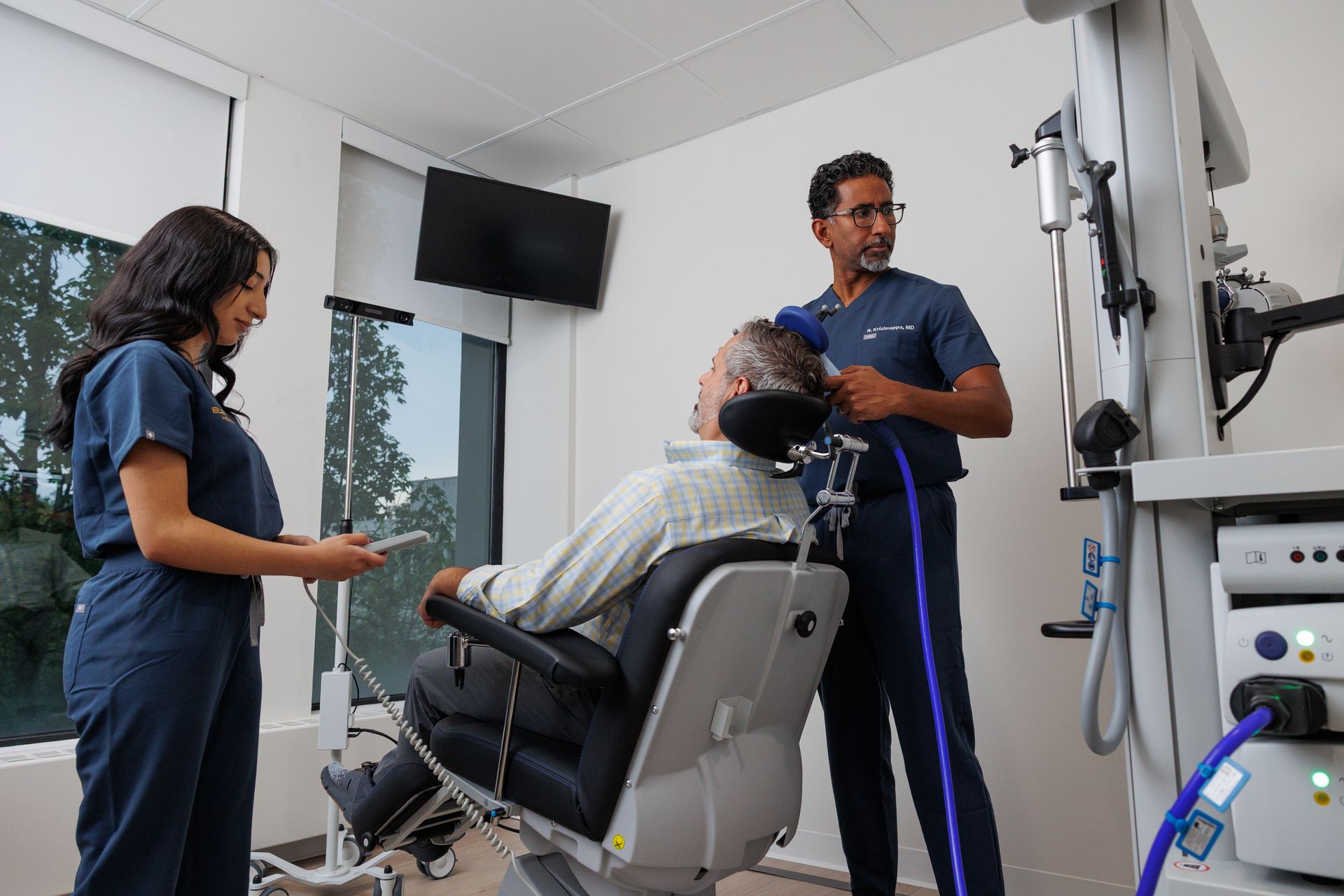
How TMS is delivered for anxiety (protocols)
There’s no single “anxiety protocol” — treatment is individualized. Common approaches include:
- Standard rTMS: repetitive pulses over the dorsolateral prefrontal cortex (DLPFC) — often used when anxiety co-exists with depression.
- iTBS (intermittent theta burst stimulation): a shorter, accelerated protocol that delivers bursts of stimulation in minutes rather than half-hour sessions. iTBS can be used in standard or accelerated formats.
- Device/target variations: Some centers tailor the exact coil position and parameters based on symptoms (for example, left vs right DLPFC targeting or medial prefrontal approaches), particularly when anxiety presents with specific network dysfunction. Device-specific programs (including deep TMS for OCD) demonstrate that coil geometry and target depth can matter for certain diagnoses.
Important: Your clinician chooses the protocol after a detailed evaluation (diagnosis, prior trials, and safety screening) and may combine TMS with psychotherapy (CBT, exposure therapy) or medication management to maximize results.
Who is a good candidate?
TMS for anxiety is usually considered for people who meet one or more of the following:
- Persistent or severe anxiety despite adequate trials of psychotherapy (for example, CBT or exposure-based treatments) and medications.
- Comorbid depression + anxiety, where standard TMS depression protocols can improve both mood and anxious symptoms.
- Occupational need for non-sedating options (e.g., first responders, safety-sensitive jobs) who want a non-systemic approach to symptom relief.
- Patients seeking accelerated care (time-limited professionals/commuters or destination patients) who can tolerate intensive schedules.
- Those who prefer to avoid medication side effects or need an additional option when medications aren’t tolerated.
Who may not be a candidate: individuals with uncontrolled seizure disorders, certain intracranial metal implants, or unstable medical conditions. Active psychosis or uncontrolled substance use would also typically require stabilization first. Clinics perform a careful medical and medication review to identify contraindications.
Read More: Is TMS Right For Me?
Typical patient profiles & examples
- GAD with partial medication response: A patient with chronic generalized anxiety who improved partially on SSRIs but still has disabling worry may benefit from TMS combined with CBT.
- Panic disorder with avoidance: When panic persists despite therapy and meds, targeted TMS plus exposure/CBT may reduce physiological reactivity and support behavioral recovery.
- Comorbid depression + anxiety: Many patients with mixed presentations respond to standard depression-targeted TMS, with concurrent reductions in anxiety symptoms.
- First responders / safety-sensitive workers: TMS offers a non-systemic path when medications are constrained by duty requirements — Elevium develops return-to-duty plans in coordination with employers and medical officers.
How results are measured
Clinics use validated outcome scales to quantify benefit: GAD-7 for generalized anxiety, PHQ-9 for depression, and CGI (Clinical Global Impression) for overall change. Treatment teams track scores regularly and adjust the plan — including boosters, maintenance sessions, or integrated psychotherapy — based on the trajectory of improvement.
Safety, side effects & monitoring
TMS is generally well tolerated. Common side effects are scalp discomfort and mild headaches that typically lessen over time. Serious risks (like seizures) are rare with proper screening and protocol adherence. Clinics screen for seizure risk, review medications that lower seizure threshold, and calibrate motor thresholds for safe dosing. Patients are monitored during and after sessions for any adverse effects.
Combining TMS with psychotherapy & medications
Best outcomes often come from an integrated approach:
- Psychotherapy (CBT/ERP) addresses the behavioral components of anxiety, while TMS can modulate the neural circuits that make therapy more effective.
- Medication management remains essential for many patients; Elevium coordinates medication changes and prior authorizations when clinic-administered treatments (e.g., Spravato) are considered. Collaboration across teams is standard practice.
Practical considerations: logistics, cost & travel
- Session cadence & time commitment: Standard courses require daily visits for several weeks; accelerated protocols compress sessions into a shorter period (useful for commuters and destination patients). Each clinic’s schedule differs, so confirm the daily time on site.
- Costs & coverage: Insurance coverage for TMS in anxiety is less established than for depression; many clinics offer benefits checks and private accelerated packages for destination care. Elevium provides itemized cost estimates, concierge scheduling, and discreet self-pay options for privacy-minded patients.
How to decide — questions to ask your clinician
- Is my anxiety diagnosis one that has evidence for TMS?
- Have I completed evidence-based psychotherapy (CBT/ERP) and adequate medication trials?
- What protocol will you use and why (rTMS, iTBS, target area)?
- What are the expected timelines and measures for success?
- What are the safety checks and contraindications in my case?
- If I’m an executive or traveling for care, what concierge/travel services do you offer?
Is TMS FDA-cleared for anxiety?
TMS has strong FDA clearance for major depressive disorder and device-specific clearances for other indications (for example, deep TMS for OCD). For anxiety disorders, research is promising and many clinics offer TMS off-label with careful clinical rationale. Your clinician will explain the evidence relevant to your diagnosis.
How soon will I notice improvement?
Some patients notice early symptom relief; others need the full course and maintenance sessions. Outcomes vary by diagnosis and history.
Can TMS replace medication or therapy?
TMS can be an effective alternative or adjunct. For many, the best results come from combining TMS with psychotherapy and, when appropriate, medication.
Are there special programs for first responders or executives?
Yes. Clinics like Elevium offer destination planning, concierge scheduling, and duty-sensitive care pathways for safety-sensitive workers and privacy-minded executives. Ask about departmental partnerships and return-to-duty planning
Share Article