Accelerated vs Standard TMS: Benefits, Time, and Outcomes

Quick answer
Both standard rTMS and accelerated iTBS use the same TMS technology to stimulate brain circuits involved in mood. Standard rTMS spreads treatment over 4–6 weeks (one session/day), while accelerated protocols compress multiple short sessions into days (e.g., 10 sessions/day × 5 days). Many patients achieve similar clinical benefits with either approach, but they differ in logistics, evidence-based maturity, and who they suit best. Clinicians pick the protocol based on clinical history, safety, time constraints, and patient preference.
What each approach is — in plain language
Standard rTMS (traditional)
- What it is: Repetitive magnetic pulses delivered once per day (typically 20–45 minutes) to a targeted brain area (commonly the left dorsolateral prefrontal cortex) for ~4–6 weeks (about 20–30 sessions).
- Why it’s used: Has a substantial evidence base and well-established insurance coverage pathways for treatment-resistant major depressive disorder. It’s often the default option when time permits and the patient prefers the conventional schedule.
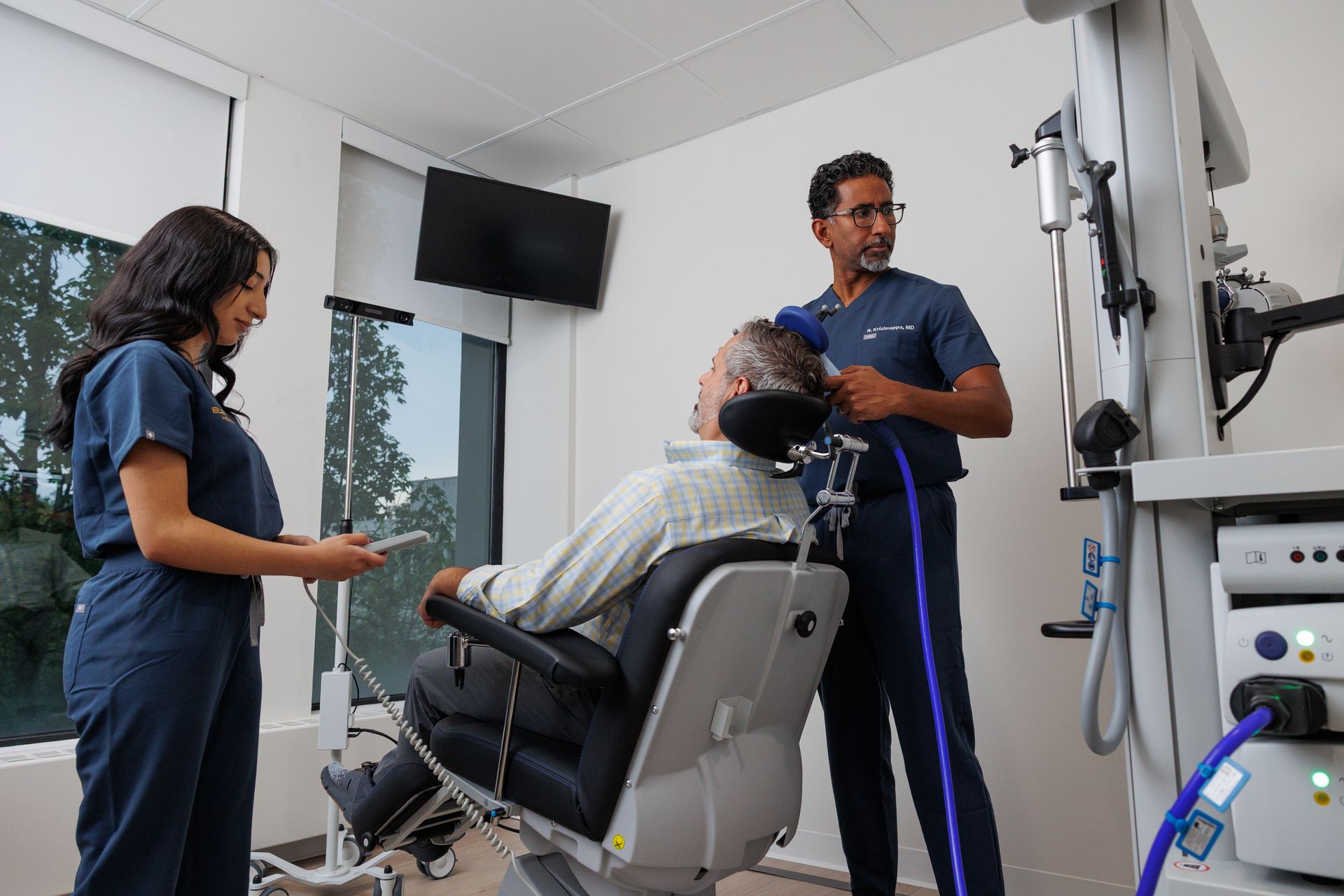
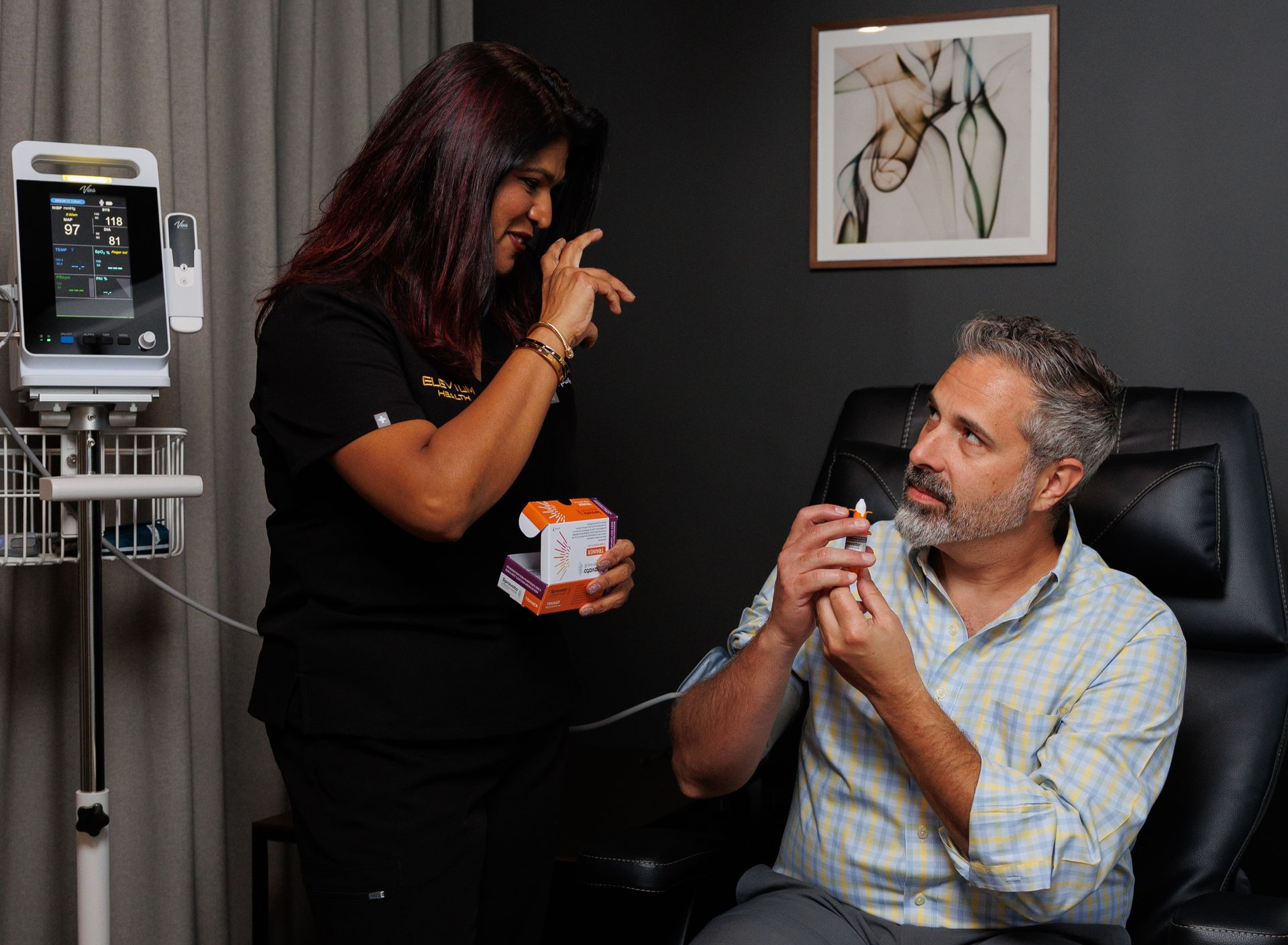
Accelerated TMS (commonly iTBS)
- What it is: Intermittent Theta Burst Stimulation (iTBS) and similar condensed protocols deliver short bursts of stimulation (often 3–10 minutes per session) multiple times per day, allowing a full therapeutic course to be completed in days rather than weeks (for example, ~10 sessions/day × 5 days ≈ 50 sessions).
- Why it’s used: iTBS is designed for faster neuroplastic change and is attractive for patients who can’t commit to weeks of daily clinic visits — busy professionals, commuters, or destination patients who travel to complete a week of intensive care. Clinics offering accelerated courses combine careful screening with scheduling and concierge logistics.
Side-by-side: benefits, time & trade-offs
| Feature | Standard rTMS | Accelerated TMS (iTBS) |
|---|---|---|
| Typical schedule | 1 session/day for 4–6 weeks (20–30 sessions) | Multiple short sessions/day for several consecutive days (e.g., 10/day × 5 days) |
| Session length | 20–45 minutes | ~3–10 minutes per iTBS session |
| Total on-site time | Short daily visits across weeks | Long clinic days (many short sessions + breaks) during treatment week |
| Evidence & approval | Large evidence base for MDD; established coverage pathways | Growing evidence; many clinics report comparable efficacy in selected patients |
| Best for | Patients who can attend weeks of treatment and prefer steady pacing | Time-limited patients, executives, commuters, destination patients |
| Insurance | More established–prior authorization often possible | Coverage variable; many clinics offer private/concierge packages |
| Tolerability | Well-tolerated; scalp discomfort/headache common | Well-tolerated; fatigue/headache possible with intensive days |
| Logistics | Easier on-site time per day | Requires planning (lodging, time off) but finishes quickly |
| Clinical flexibility | Easy to combine with weekly therapy | Often combined with intensive scheduling and concierge support |
Outcomes — what the evidence and real-world data show
- Efficacy: Standard rTMS has robust randomized controlled trial evidence for major depressive disorder. Accelerated iTBS has shown promising results in trials and real-world practice, with many centers reporting comparable response and remission rates in selected patients. Evidence is still expanding, but accelerated protocols can produce clinically meaningful improvement faster for many people. Clinicians assess response using standardized scales (PHQ-9, GAD-7, CGI) and tailor follow-up plans.
- Durability: For both approaches, some patients achieve durable remission, while others need maintenance sessions or boosters. Long-term outcomes can be improved by combining TMS with psychotherapy and medication management.
Who is a better fit for each option?
Consider Standard rTMS when:
- You can attend daily visits for several weeks.
- You prefer the more established protocol with broad insurance coverage.
- You have comorbidities that favor more conservative pacing or closer monitoring over time.
Consider Accelerated TMS when:
- You have time constraints (work, caregiving) and cannot commit to a 4–6 week course.
- You are an executive, commuter, or destination patient who can arrange a single treatment week with lodging near the clinic.
- You prefer a condensed plan and are willing to accept longer clinic days in exchange for finishing quickly.
- Your clinician judges that an accelerated protocol is clinically appropriate for your diagnosis and safety profile.
Safety & monitoring - same priorities, different rhythms
Safety principles are identical: screen for seizure risk, review implants and medications, calibrate motor threshold, and use trained staff and protocols. Accelerated programs add considerations about day-long fatigue and cumulative short-term effects from multiple sessions, so clinics monitor patients closely throughout each day. Seizures remain rare when protocols and screening are followed.
Practical factors: logistics, cost & travel
- Time & daily rhythm: Standard rTMS spreads time burden across weeks; accelerated TMS concentrates it into intensive days. Which is better depends on your life responsibilities.
- Travel & destination care: Accelerated protocols are ideal for destination patients; Elevium and similar clinics provide concierge travel packs, lodging suggestions, and private scheduling to make a treatment week feasible for out-of-state or executive patients. If traveling, plan to arrive the night before Day 1 and add a buffer before flying home.
- Cost & insurance: Standard rTMS typically has clearer PA pathways and insurer precedent; accelerated packages are often offered as private or self-pay bundles. Ask clinics for itemized estimates and benefits checks.
How clinicians choose — decision factors
Clinicians weigh:
- Clinical history — prior treatment failures, comorbidities, severity.
- Safety profile — seizure risk, implants, medications.
- Function & logistics — patient’s ability to attend many short sessions vs spread-out sessions.
- Evidence & local expertise — some clinics have more experience with accelerated protocols.
- Patient preference — willingness to travel, privacy needs, tolerance for long clinic days.
A shared decision-making process explains trade-offs and sets expectations for outcomes and maintenance.
Are outcomes really the same for accelerated and standard TMS?
Many studies and clinic series show comparable outcomes for selected patients, but results vary across individuals and protocols. Your clinician will review the evidence relevant to your case and recommend the best option.
Is accelerated TMS more likely to cause side effects?
Accelerated regimens can cause transient fatigue because of long clinic days, but most side effects (scalp soreness, headaches) are similar and manageable. Close monitoring is essential.
Does insurance cover accelerated TMS?
Coverage for standard TMS is more established; accelerated packages are frequently offered as private bundles. Clinics can run benefits checks and attempt prior authorizations, but patients should expect variable coverage.
Can I switch from one protocol to the other?
Yes — clinicians sometimes start with one approach and modify plans based on tolerance and response. Maintenance or booster sessions can be adjusted over time.
Share Article