Prepare for Your First TMS Session: A Practical Checklist

Quick overview
Your first TMS visit is an important step — and a little preparation makes it smooth. This guide walks you through exactly what to do before, on the day of, and after your first Transcranial Magnetic Stimulation (TMS) session so you arrive prepared, reduce anxiety, and speed your path to care. If you’re traveling or want private scheduling, see the concierge note at the end.
Complete your intake BEFORE you arrive (do this first)
- Finish the forms in the Tebra Patient Portal. This is the fastest way to upload medication lists, records, consent forms, and any questionnaires the clinic uses. Elevium puts the Tebra link in the top navigation — please use it before you visit speed screening and check-in.
- Send recent records. Upload recent psychiatric notes, medication lists (dose & dates), and any relevant lab results or imaging. If you don’t have records, ask your prior clinician for a summary.
- Complete a telehealth pre-screen (if offered). Many clinics do a brief tele-visit to review history and answer questions before in-person titration.
Confirm medical screening & clearance
- Seizure & implant screening. TMS requires a safety review for seizure history and intracranial metal/implants. Be honest about any prior seizures, head trauma, or metal hardware. Seizures are rare with proper screening and protocol adherence.
- Medication review. Bring a full list of current medications (including OTC and supplements). Some meds affect seizure threshold and may require temporary adjustment. Your prescribing clinician will advise.
- Medical clearance (if needed). If you have cardiac issues, uncontrolled hypertension, or other complex medical conditions, your clinic may request clearance from your PCP or cardiologist.
Practical checklist - what to bring
- Photo ID and insurance card (if using insurance).
- A printed or digital medication list (drug name, dose, frequency).
- Completed intake forms from the Tebra Patient Portal (bring confirmation or screen shot).
- Comfortable, layered clothing (temperature in clinics varies).
- Snacks and a water bottle for between sessions.
- Phone charger, headphones, or reading material for breaks.
- Emergency contact/escort info if your clinic recommends it (most TMS do not require a driver, but check clinic guidance).
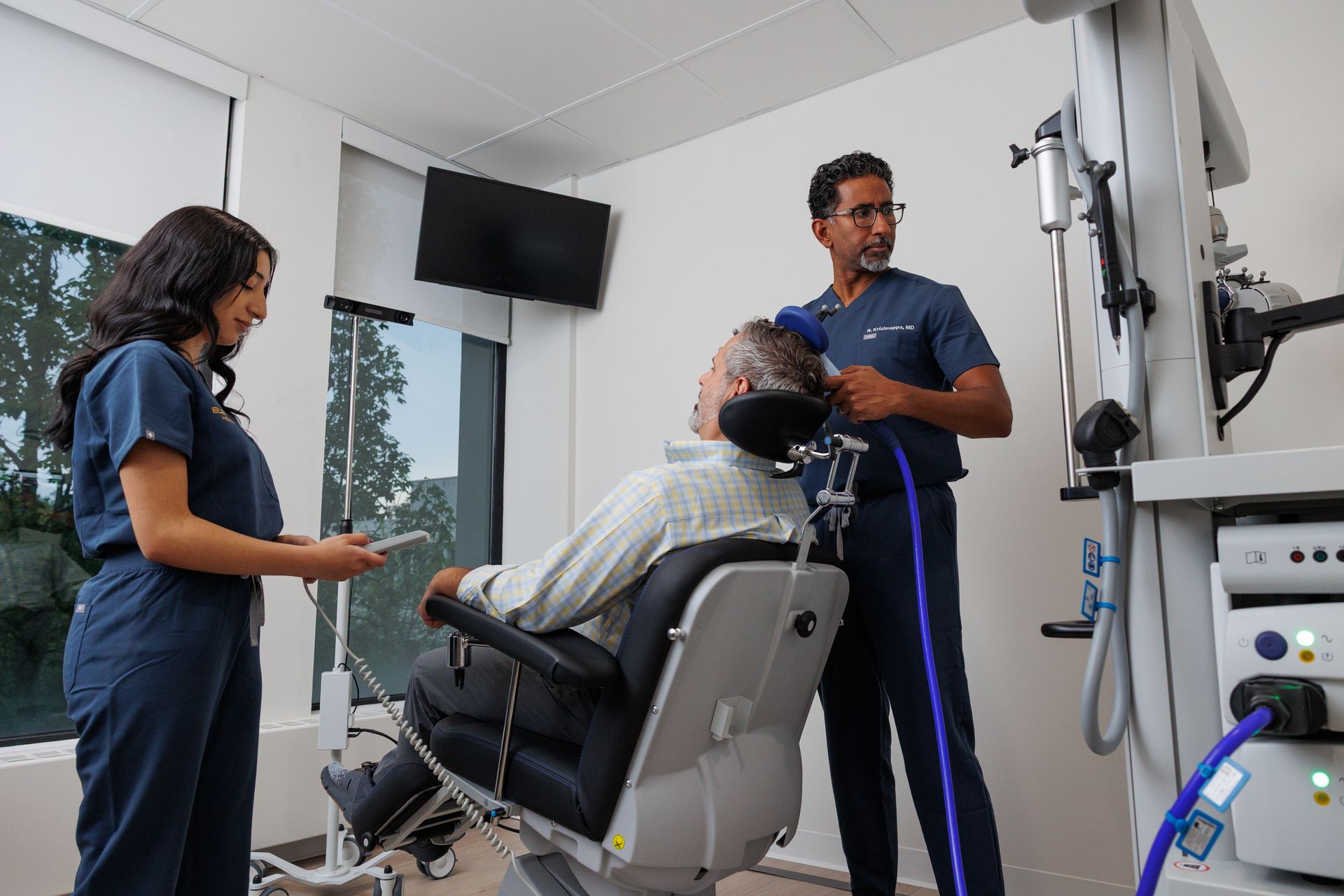
What to expect on your first session (timeline)
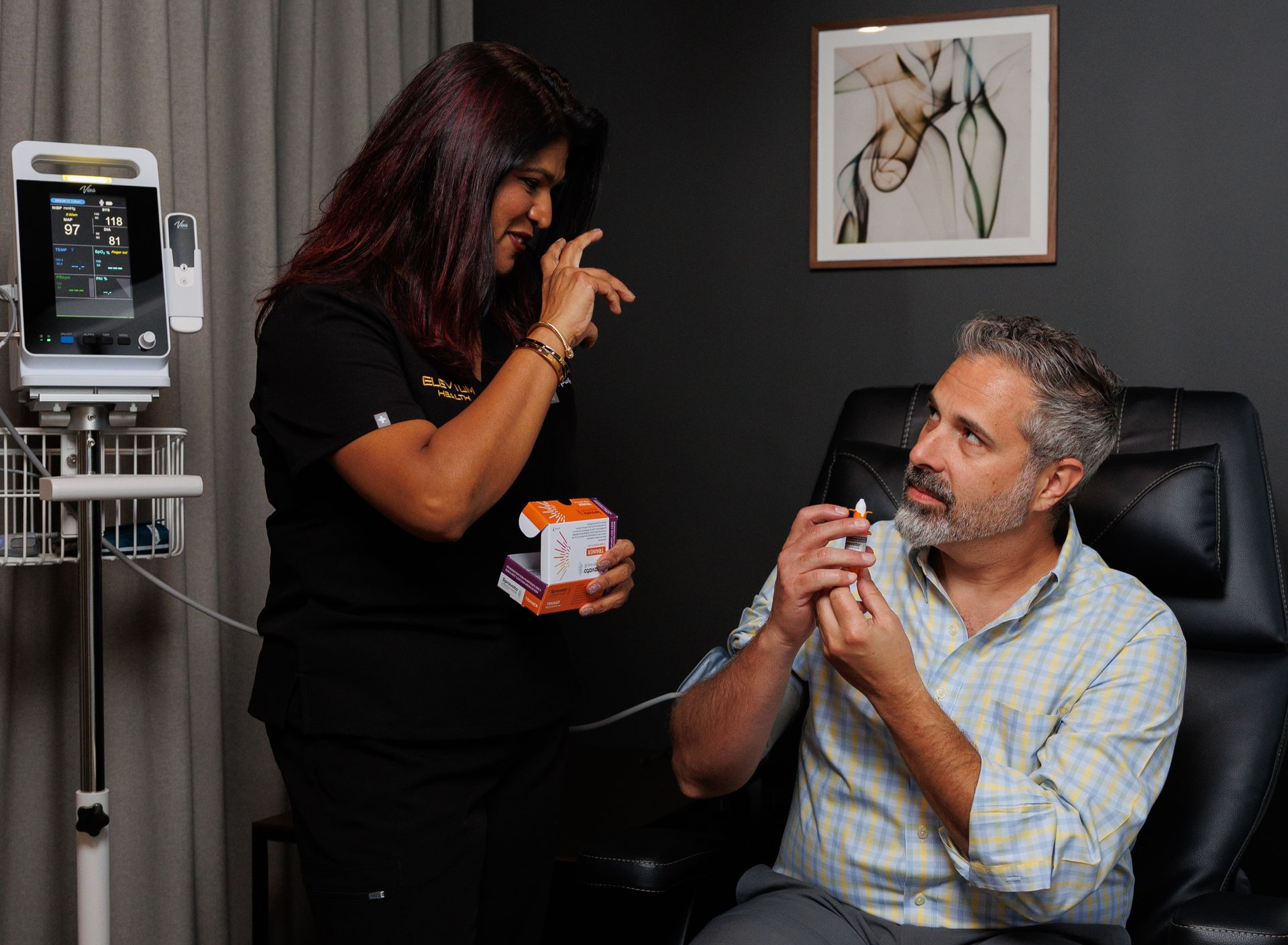
Arrival & check-in (10–20 minutes)
Sign the consent forms (if not completed), confirm your medical history, and have vitals taken.
Psychiatric intake & consent review (30–60 minutes)
A clinician reviews diagnosis, meds, benefits/risks, and answers questions.
Motor threshold titration (30–60 minutes)
A short calibration procedure finds the appropriate stimulation intensity for you. This ensures dosing is safe and personalized.
First stimulation block (varies, often <30 minutes)
You’ll experience tapping on the scalp. Technicians monitor your comfort frequently. Headache or scalp discomfort can occur and usually improves.
Post-session check & scheduling (10–15 minutes)
Clinician reviews how you felt and schedules follow-ups. For accelerated programs, you’ll get the daily schedule for upcoming sessions.
Day-of tips to feel your best
- Eat a light meal before arriving — avoid heavy or greasy foods that make you sluggish.
- Hydrate well the day before and the morning of treatment.
- Avoid alcohol 24 hours before your session.
- Pace yourself between sessions with short walks, stretching, or quiet relaxation.
- Bring OTC pain relief (ibuprofen or acetaminophen) only if approved by your clinician for headaches.
Aftercare & the first 24–48 hours
- Mild headache or scalp soreness is common — usually improves quickly.
- Fatigue: You may feel tired; plan light activity the rest of the day.
- Report any unusual symptoms immediately (severe headache, visual changes, new weakness, or confusion). Clinics provide emergency guidance.
- Follow-up: expect a scheduled check-in within 1–4 weeks to monitor response and plan the course (or maintenance) as needed.

Special notes for accelerated / destination patients & executives
- Concierge & travel planning: If you’re traveling for an accelerated TMS week or need private scheduling, ask about the clinic’s Destination Patient Coordinator or concierge services — they can arrange travel itineraries, lodging, and discreet billing. Elevium’s model uses the Tebra portal and concierge support to make destination care seamless.
- Time management: Accelerated days can be long (multiple short sessions separated by breaks). Plan your travel/lodging within a short walk/drive of the clinic and arrive the night before for the best rest.
Insurance & costs - what to check beforehand
Benefits check: Ask the clinic to run a benefits check and estimate out-of-pocket costs before your first visit. Standard TMS often has prior-authorization pathways; accelerated/intensive packages are frequently self-pay. Elevium routinely performs PA submissions and provides itemized estimates.
Will TMS hurt?
Most patients feel tapping or mild discomfort at the scalp. Headaches are common early and usually resolve with simple measures.
Do I need someone to drive me home?
TMS does not usually require sedation, and most patients can drive. Follow your clinic’s guidance; accelerated days can be tiring and an escort may be recommended if you feel fatigued.
How long until I see improvement?
Many patients do, but clinics often recommend a buffer day if possible - ask your care team.
Is TMS safe?
Yes - when performed by experienced teams with proper screening and motor-threshold calibration. Seizures are rare with correct protocols.
Share Article