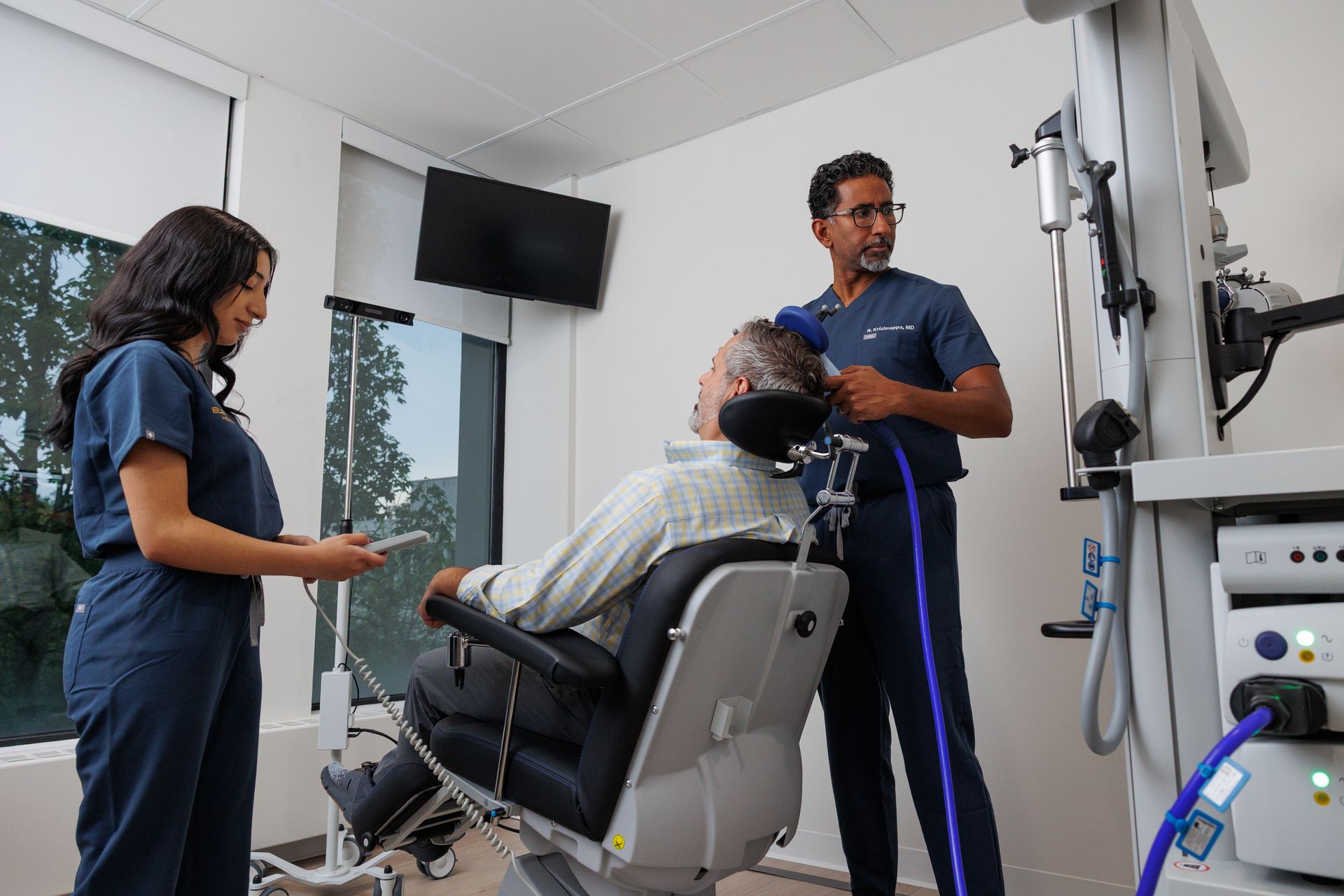
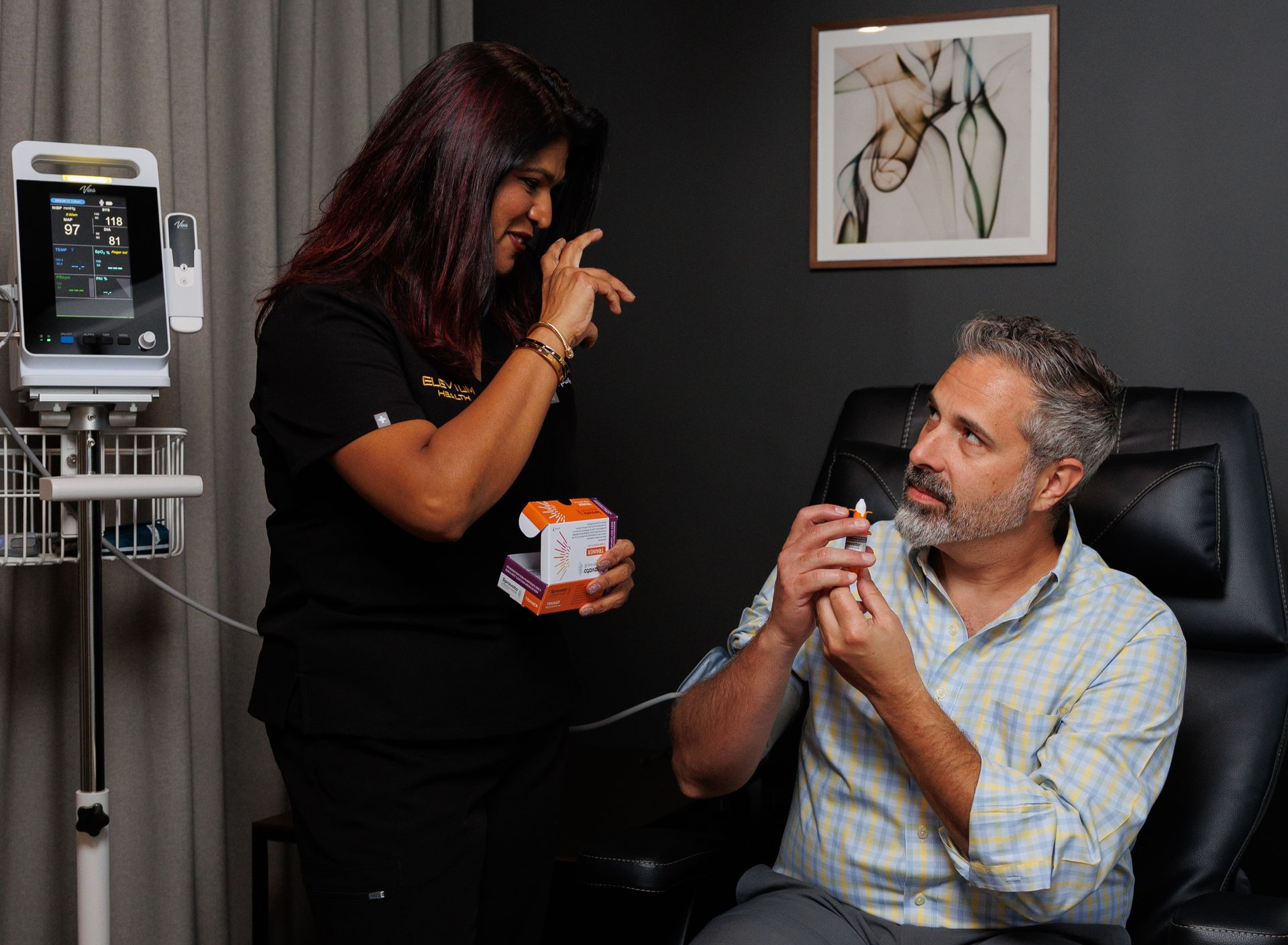
TMS for First Responders & Public Safety Workers

Why this matters
First responders and public safety workers face unique clinical and occupational constraints: certain medications can impair alertness or reaction time, and some roles (firefighters, police officers, air-crew) require careful consideration of fitness for duty. TMS is a non-systemic, non-sedating intervention that can be an important treatment option when medication choices are limited by duty requirements. Elevium’s model supports duty-sensitive care, departmental outreach, and return-to-duty planning to help workers recover safely while maintaining public safety.
Key clinical advantage: non-systemic option
TMS is non-systemic — it does not require daily oral medication and does not carry the same systemic side effects (sedation, slowed reaction time) that can limit occupational fitness. Because TMS stimulates target brain circuits externally, many first responders tolerate it without effects that would interfere with duty. This makes TMS an attractive alternative or adjunct when medications are contraindicated for work reasons.
Medication limitations & common duty concerns
Many commonly used psychiatric medications may pose challenges for safety-sensitive occupations:
- Sedative medications (benzodiazepines, sedating hypnotics) can impair judgment, alertness, and motor skills — often disqualifying for duty.
- Certain antidepressants can cause sedation, orthostatic hypotension, or slowed reaction time in some patients, which requires monitoring.
- Medications that alter cognition or cause profound fatigue are generally avoided or used with caution in active duty roles.
- Controlled substances and substances that affect performance may require special workplace policies and monitoring.
Because of these constraints, departments often seek non-pharmacologic options or medication regimens that preserve alertness and safety. Elevium’s medication-management team works closely with occupational medical officers to find duty-compatible plans and to document clinical rationale when medications are necessary.
Evidence & candidate profiles
Who might benefit
- First responders with major depressive disorder or co-occurring anxiety who either cannot tolerate standard medications or have occupation-related medication restrictions.
- Workers with treatment-resistant symptoms despite therapy and limited medication options.
- Personnel seeking a non-sedating, evidence-based treatment option that can be coordinated with employers.
Evidence
TMS has a robust evidence base for major depressive disorder and growing support for anxiety and other comorbid conditions. While device protocols differ (standard rTMS, iTBS, deep TMS for specific diagnoses), many clinics have successfully adapted TMS pathways for duty-sensitive workers with careful screening and coordination. Outcomes are measured with standardized scales, and return-to-duty readiness is evaluated case-by-case.
Practical duty considerations & return-to-duty planning
Screening & medical clearance
- Medical and medication review (seizure history, implants, cardiovascular risk).
- Coordination with occupational medicine or department medical officers for fitness-for-duty assessment.
On-treatment monitoring
- TMS requires no systemic anesthesia; most patients resume normal activity after sessions. Clinicians still evaluate fatigue or headaches that may temporarily affect duty readiness.
- For accelerated protocols (condensed schedules), plan for potential short-term fatigue during the treatment week. Departments may prefer light duty for intensive days.
Return-to-duty steps
- Documented clinical improvement using validated scales (PHQ-9, GAD-7, CGI).
- Occupational assessment by department medical officer, incorporating clinician notes and functional status.
- Stepwise clearance — phased or modified duty as needed (e.g., limited-field assignments, no heavy equipment) with re-evaluation intervals.
- Maintenance & follow-up — booster TMS sessions or ongoing psychotherapy/medication as clinically indicated.
Elevium develops return-to-duty plans in partnership with departments to balance recovery and public safety.
Alternatives & complementary pathways
- Standard TMS (daily sessions over weeks) — useful when time allows and for stable schedules.
- Accelerated TMS / iTBS — condensed options for time-limited workers or destination patients; requires planning for daily onsite time and possible short-term fatigue.
- Psychotherapy (CBT/ERP) — essential for anxiety/PTSD and to consolidate gains from TMS.
- Careful medication strategies — where medications are necessary, choice and dosing are customized to minimize duty impairment; occupational restrictions are explicitly addressed.
- Spravato / ketamine — these options can have rapid effects but require in-clinic monitoring (Spravato REMS — ≥2 hours observation) or may cause dissociation; they may be unsuitable for immediate return to duty and often require careful clearance.
Departmental outreach & partnership playbook
To make TMS workable for departments, Elevium recommends a structured partnership approach:
1. Department packet (what to include)
- Clinical overview of TMS & iTBS (mechanism, evidence).
- Candidate criteria and contraindications.
- Sample return-to-duty workflow and clearance checklist.
- Itemized pricing & benefits check overview for common insurers & self-pay packages.
- Privacy & documentation protocols.
- Contact information for a dedicated Department Coordinator at Elevium.
2. Outreach steps
- Intro call with department leadership (HR/Medical Officer).
- Educational briefing: 30–60 minutes in-service explaining TMS, duty implications, and case examples.
- Case consultation: confidential review of referred employees with appropriate releases.
- Create referral pathway: secure referral form, expedited scheduling, and occupational follow-up templates.
3. Operational details to agree
- Data-sharing/consent procedures for fitness-for-duty notes.
- Expected turnaround for evaluations and treatment scheduling.
- Reporting cadence and KPIs (referrals processed, time to evaluation, successful return-to-duty).
Will this affect my ability to carry a weapon or operate machinery?
TMS itself is non-systemic and usually does not impair ongoing duties. Clearance must be individualized; in some cases temporary duty modification may be recommended during intensive treatment days. Elevium works with departments to document fitness appropriately.
How long before I can return to full duty?
Return depends on symptom improvement and functional assessment; many cases use stepwise clearance with objective measures and occupational input.
Is TMS covered by insurance for employees?
For treatment-resistant depression, many insurers will cover standard TMS with prior authorization. Accelerated/destination programs often use private packages. Elevium performs benefits checks and provides itemized cost estimates.
Share Article