What To Ask During Your First Consultation
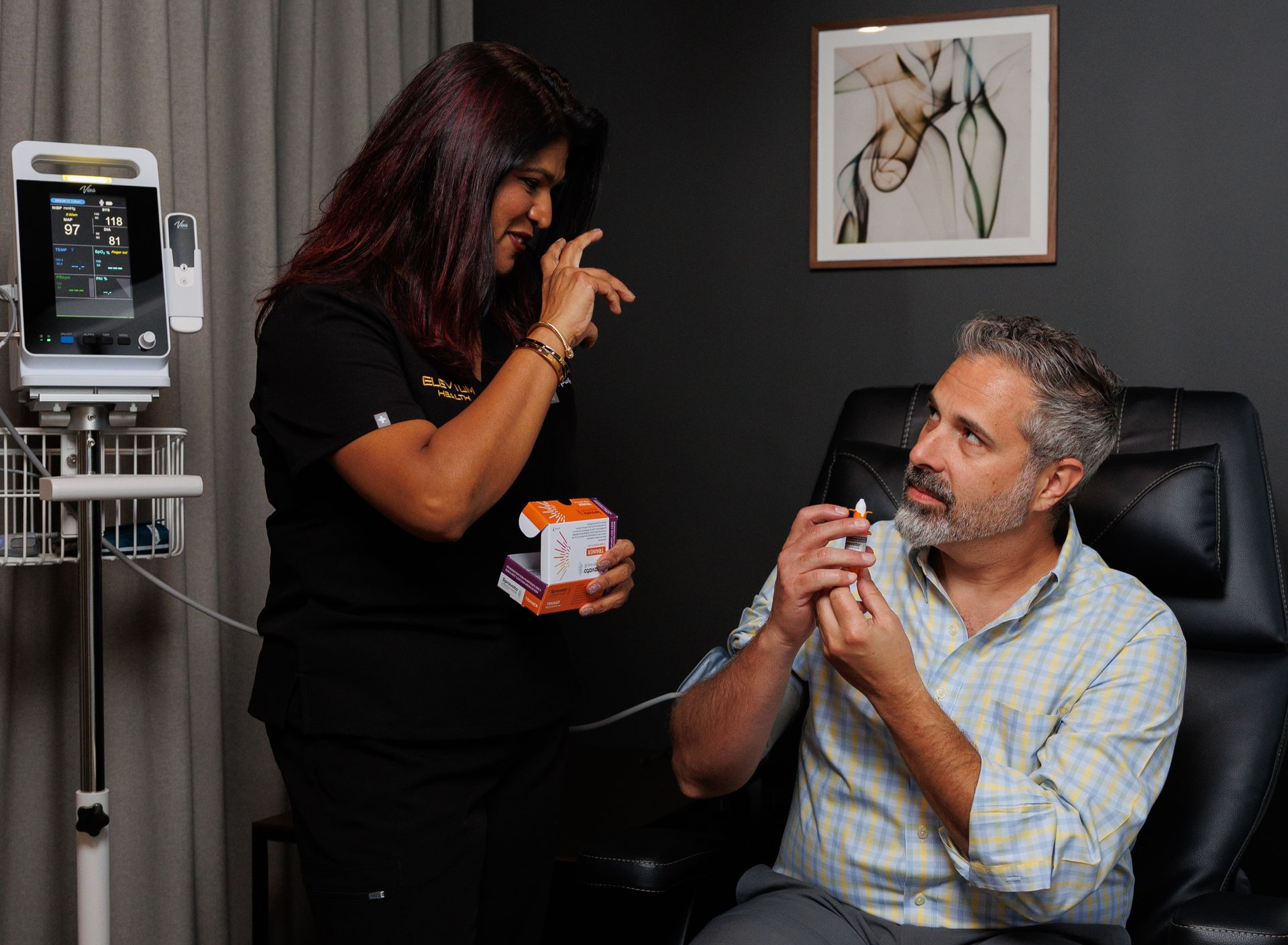
A first consultation for Transcranial Magnetic Stimulation (TMS) or ketamine therapy is an important conversation - not just about the treatment itself, but about your goals, safety, logistics, and costs. Use this 20-item checklist to make the most of your visit. For each question below, we explain why it matters and what a clear answer might sound like.
Questions about eligibility & clinical fit
Am I a good candidate for this treatment?
Why: Candidacy depends on diagnosis, treatment history and medical risks.
What to expect: The clinician should review your psychiatric and medical history and explain why TMS or
ketamine is (or isn’t) appropriate.
What evidence supports this treatment for my condition?
Why: You should hear about clinical outcomes and the strength of evidence for your diagnosis.
Good answer: A clinician references studies or guidelines, and explains expected response rates and what success looks like for your condition.
Have I tried other recommended treatments first?
Why: Many protocols call for prior trials of therapy/medication before advanced options.
What to expect: A review of past medications, psychotherapy, and reasons you’re considering TMS/ketamine now.
Are there medical risks or reasons I should not receive treatment?
Why: Safety screening (seizure risk, implants, cardiovascular issues) is critical.
Good answer: The team will ask focused medical questions and describe contraindications and monitoring plans.
How do you determine the exact protocol (dose, number of sessions)?
Why: Protocols differ (standard vs accelerated TMS; oral/IM/IV ketamine). You should understand selection logic.
What to expect: Clinicians explain motor threshold testing (TMS), session frequency, or ketamine route and dosing rationale.
Will I need anything else alongside this treatment (therapy, meds)?
Why: Combining TMS or ketamine with psychotherapy or medication often improves outcomes.
Good answer: A recommendation for follow-up therapy (often CBT) or medication adjustments as part of a treatment plan.
Questions About the Treatment Process & Experience
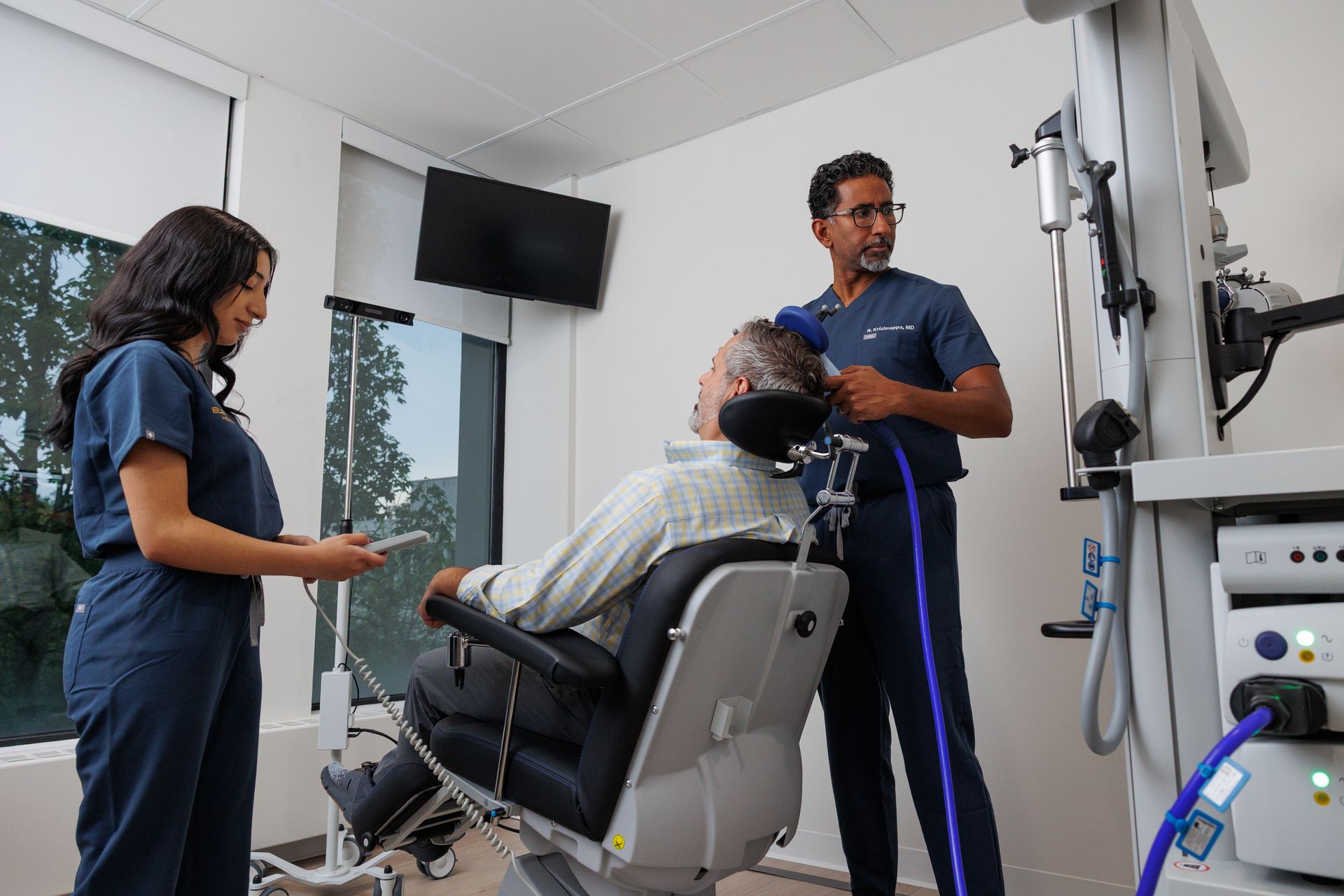
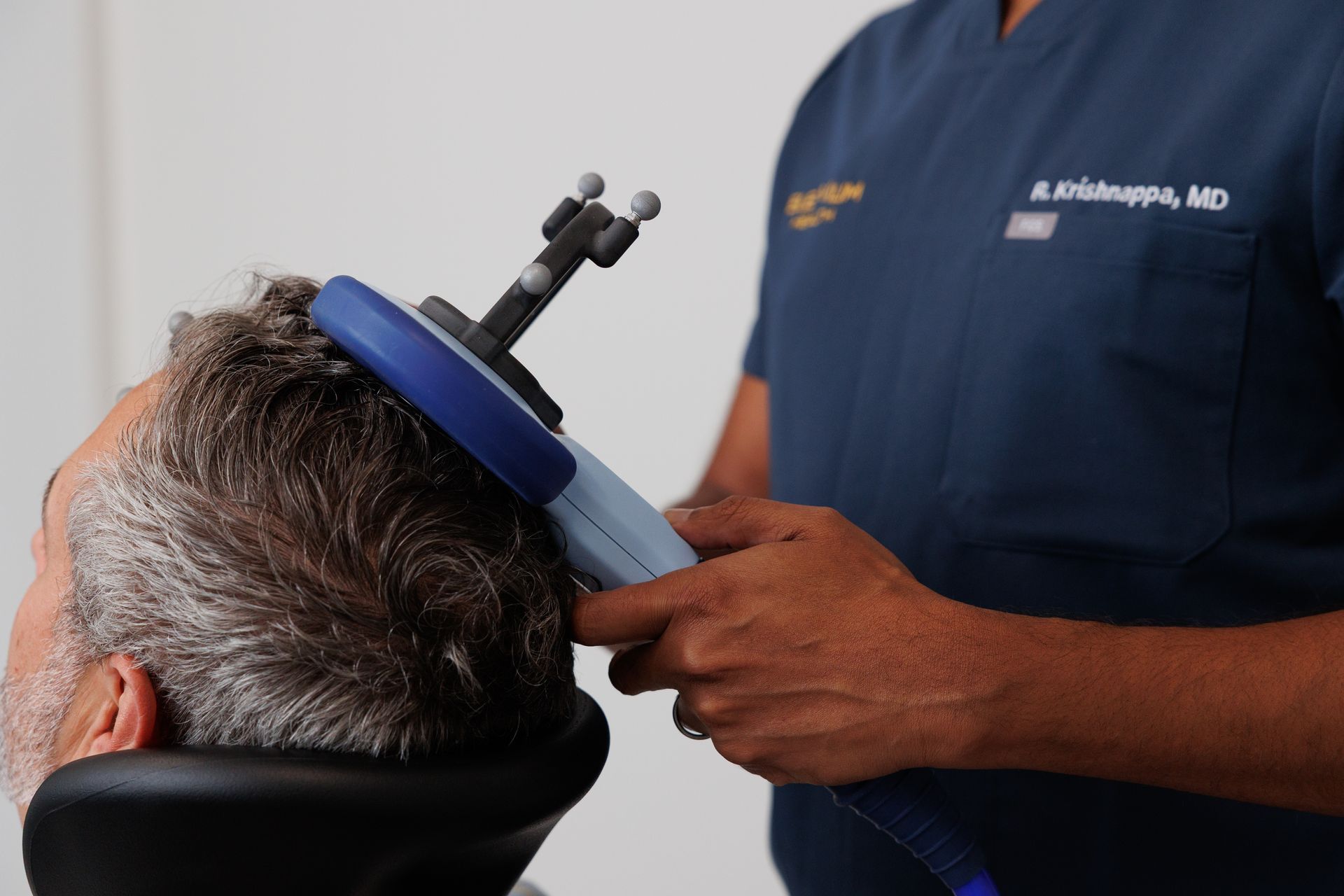
What happens during a typical session?
Why: Knowing the step-by-step experience reduces anxiety and sets expectations.
Good answer: For TMS: chair placement, motor threshold test, ~20–40 minutes of stimulation. For ketamine: route (oral/IM/IV), monitoring time and recovery expectations.
How long is a full course, and how quickly might I notice improvement?
Why: Timing affects scheduling and realistic expectations.
What to expect: Standard TMS typically spans weeks;
accelerated TMS is condensed. Ketamine courses vary by route; some patients notice quicker effects, but individual responses vary.
What are the common side effects, and how are they managed?
Why: Informed consent requires knowing likely side effects and their management.
Good answer: Mild scalp soreness/headache for TMS; transient dissociation, nausea, or blood pressure changes for ketamine — with monitoring/medications available.
How will you monitor safety during and after treatment?
Why: Safety protocols and emergency procedures matter, especially for ketamine infusions and intensive TMS programs.
What to expect: Continuous observation during sessions, vital sign checks, and post-session recovery monitoring.
What is your plan if treatment doesn’t work or causes problems?
Why: Understand fallback options, appeals, or alternative pathways.
Good answer: Clear alternatives (adjust protocol, boosters, combine with therapy, or consider different modalities).
Logistics, Scheduling & Travel
How often and when will I need to come in? Can my schedule be accommodated?
Why: Daily or multiple-daily sessions may be required; planning is essential.
What to expect: Exact schedule options, evening/weekend availability and support for commuters. (Elevium supports NYC commuter logistics.)
If I’m traveling for an accelerated course, do you help with lodging/booking?
Why: Condensed accelerated programs often require short-term stays.
Good answer: Clinic offers travel guidance and can help coordinate appointment blocks for minimal disruption.
What should I bring to my first appointment?
Why: Being prepared speeds the visit and improves safety.
Examples: ID, list of medications, prior records, insurance card (if applicable), a driver if ketamine is IV/IM and you cannot drive post-session.
Costs, insurance & payment
How much will this likely cost and will my insurance cover it?
Why: Clarify out-of-pocket expectations before committing.
Good answer: The team explains self-pay pricing vs insurance pathways and offers to verify benefits and provide a written coverage-based estimate. (Elevium verifies coverage and issues estimates.)
If insurance doesn’t cover it, what are self-pay options and payment plans?
Why: Understand deposit, installments, CareCredit and package discounts.
What to expect: Clear self-pay rates, deposit policy, and financing options.
What costs might still be billed after treatment (unexpected services)?
Why: Confirm common ancillary charges (labs, facility fees, prescriptions).
Good answer: An itemized estimate including possible add-ons and clear billing contacts.
Outcomes, follow-up & long-term plan
What are realistic outcome measures and follow-up plans?
Why: Know how success is measured and what maintenance looks like.
What to expect: Criteria for response/remission, timelines, booster options, and routine follow-up visits.
How will you measure and track my progress?
Why: Objective measures (rating scales, clinician assessments) help evaluate benefit.
Good answer: Use of standardized scales, session notes, and progress meetings scheduled at set points.
What’s the plan for aftercare and relapse prevention?
Why: Long-term maintenance matters; many patients combine therapy, boosters, or medication adjustments.
Good answer: A follow-up schedule, referral to psychotherapy, and a plan for booster sessions if needed.
How long does a consult take?
Typically 45–90 minutes for a full medical and psychiatric evaluation plus Q&A.
Do I need a referral?
Some insurers require referrals/prior authorization — the clinic can verify and assist.
Can I combine TMS and ketamine?
Combining treatments is individualized and depends on clinical rationale; discuss it with your clinician.
Share Article