Do I Need Therapy Alongside TMS or Ketamine? What Elevium Recommends
It's one of the first questions many patients ask once they've decided to pursue TMS or ketamine:
Do I need to be in therapy at the same time?
The short answer is no, it's not a requirement. TMS and
ketamine are both effective as standalone treatments. But the longer answer is more interesting, and for many patients, more useful.
What TMS and Ketamine Do, and What They Don't
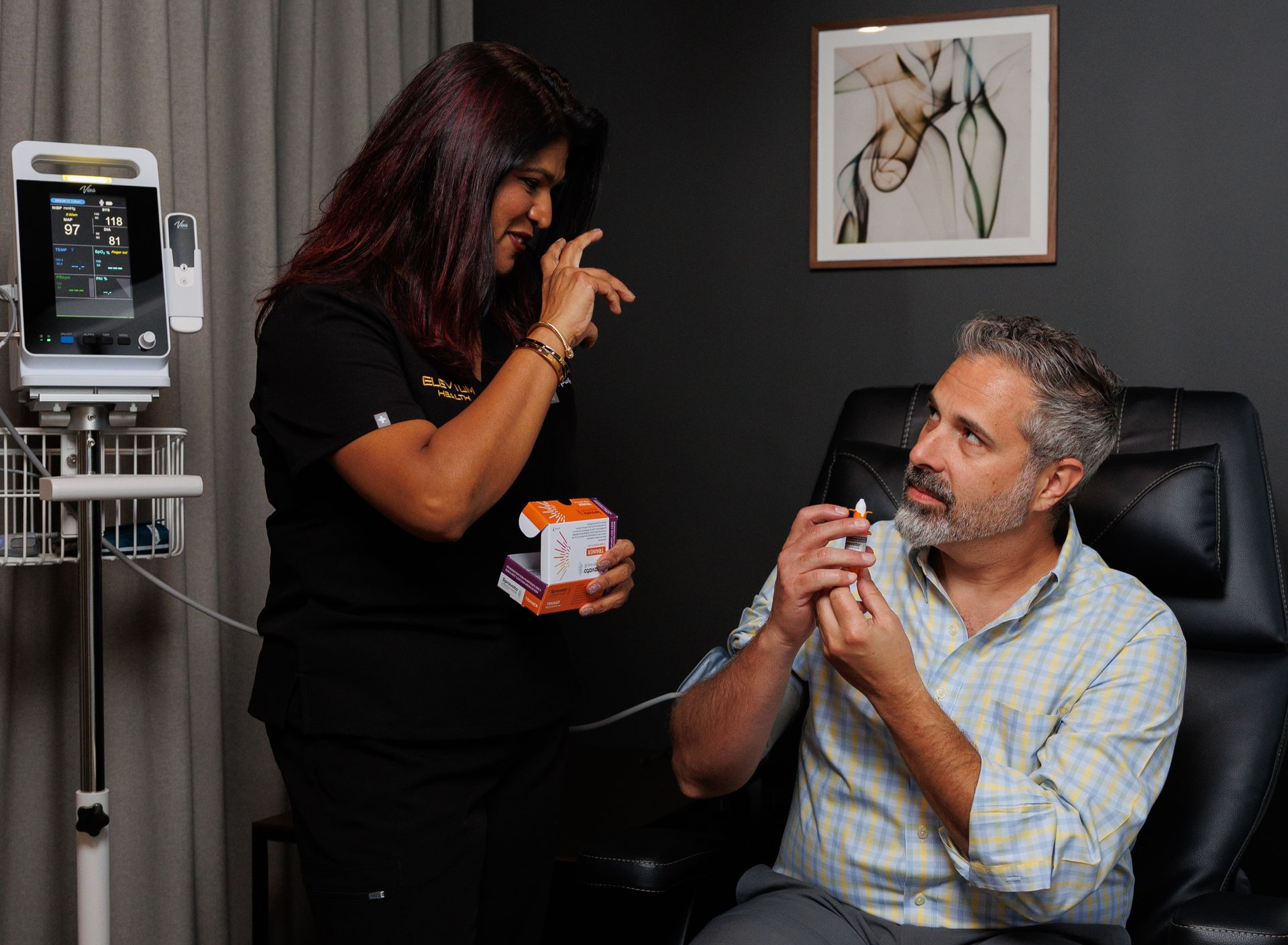
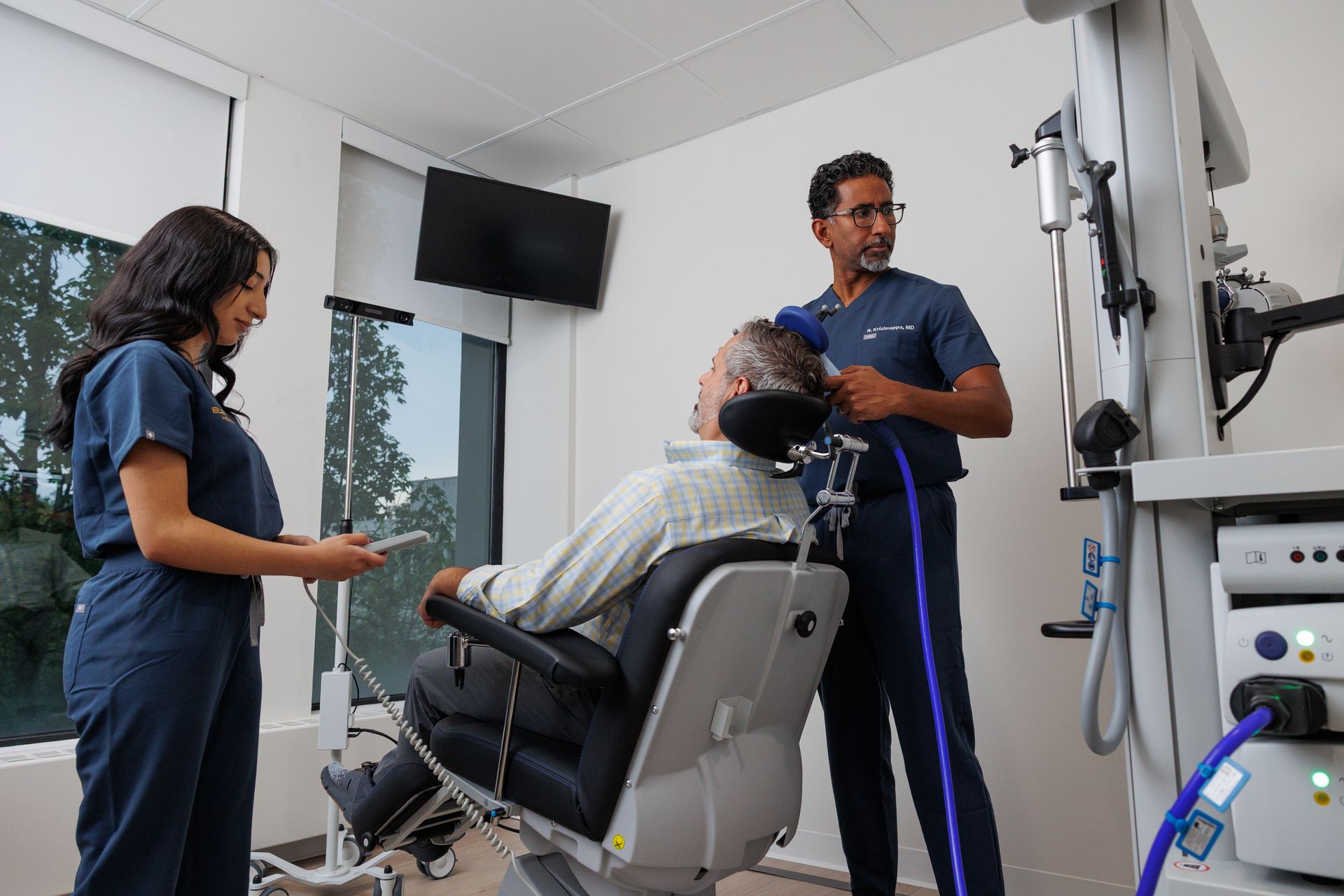
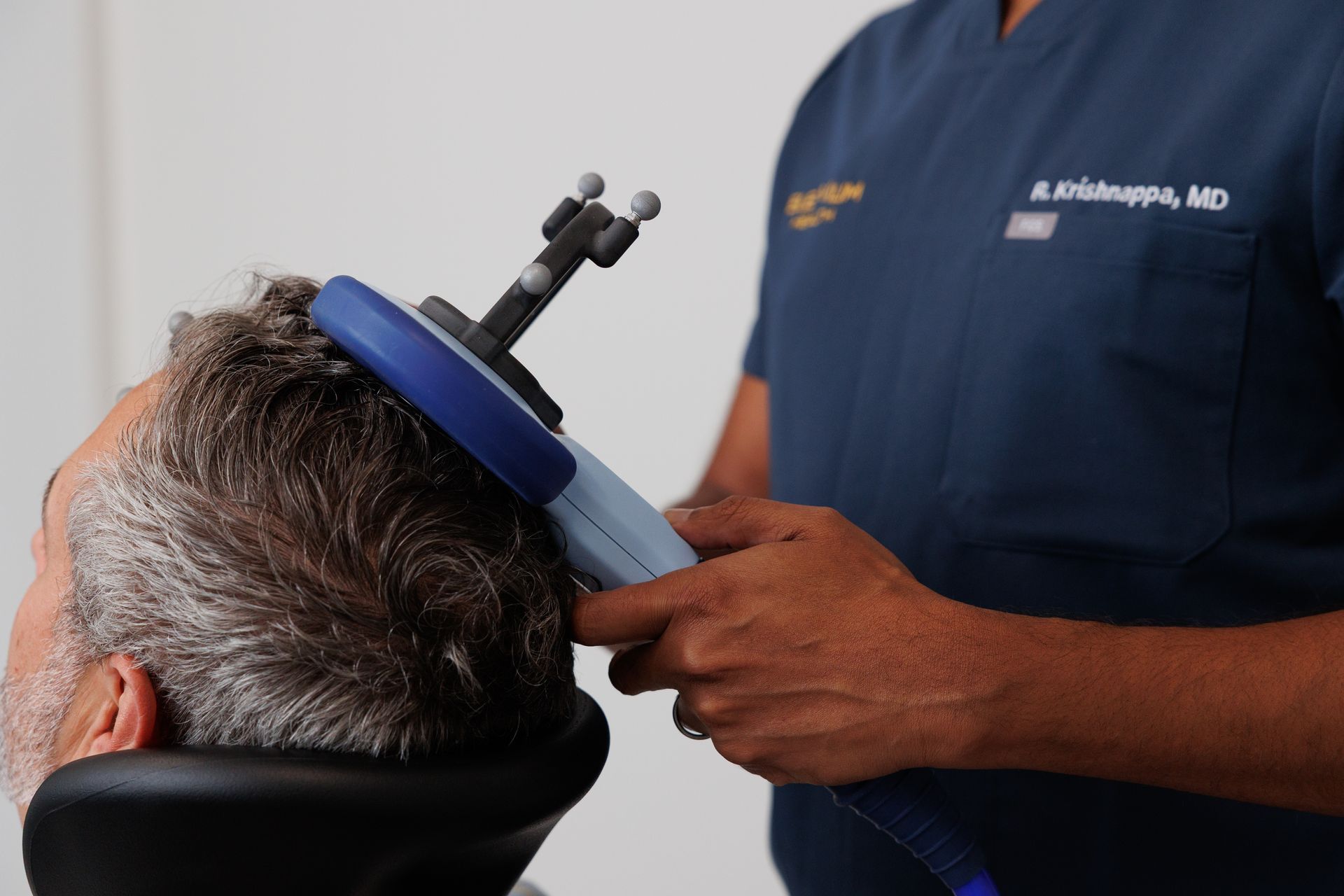
TMS and ketamine work at a neurological level. TMS uses electromagnetic pulses to modulate activity in targeted brain regions. Ketamine and Spravato act on the glutamate system, promoting neuroplasticity, the brain's ability to form new neural connections. Both can produce meaningful symptom relief, sometimes quickly.
What they don't do is address the behavioural patterns, thought processes, and environmental factors that often sit alongside depression, OCD, anxiety, or trauma. They can lift the neurological weight of a depressive episode. They can't, on their own, help you understand why certain situations trigger you, or build the coping skills to manage them.
That's what psychotherapy does.
The Case for Combining Them
There's a reason clinicians often describe ketamine and TMS as "opening a window." The neuroplasticity effects, particularly with ketamine and Spravato, create a period where the brain may be more receptive to change. Some research suggests this window is an especially valuable time to engage in therapy, because the psychological work can take root more effectively when the neurological environment is more flexible.
Think of it this way: TMS or ketamine can reduce the symptoms that make functioning difficult. Therapy can help you build the skills and insight to sustain that improvement long-term.
At Elevium, we offer CBT and DBT alongside our TMS, ketamine, and Spravato programmes. CBT helps patients identify and reframe cognitive patterns driving their symptoms. DBT adds a focus on mindfulness and acceptance, particularly useful for patients dealing with emotional dysregulation or complex trauma histories. We also offer Interpersonal Therapy and Person-Centred Therapy depending on individual need.
When Therapy Alongside Treatment Makes the Most Sense
There's no single answer that applies to everyone, but therapy tends to add the most value in these situations:
You have identifiable psychological or environmental contributors. If your depression or anxiety is tied to specific patterns, relationships, thought habits, trauma history, or chronic stress, therapy gives you tools to address those directly. TMS or ketamine alone won't resolve them.
You want to protect long-term gains. Symptom relief from TMS or ketamine can be significant, but it's not always permanent. Patients who build psychological coping skills during or after a treatment course often find their improvements last longer and that they're better equipped to manage if symptoms return.
You're working through trauma. TMS and ketamine can ease the weight of trauma-related symptoms. But processing the trauma itself, the memories, meaning, and behavioural responses- requires therapeutic work. For PTSD and related presentations, combining treatments is often the stronger approach.
You're using ketamine and want to deepen the therapeutic gains. Some patients pursuing ketamine therapy choose to integrate psychotherapy alongside the treatment course, working with a therapist to process insights that emerge during or after sessions. This is an emerging approach with a growing evidence base, particularly for treatment-resistant presentations. We can discuss whether this kind of integration makes sense for you during the consultation.
When Standalone Treatment Is Reasonable
There are also patients for whom TMS or ketamine alone is entirely appropriate, at least to start.
If you've been in therapy before and have a solid set of coping tools, adding psychotherapy during a TMS course may not be necessary. If your priority is stabilising symptoms quickly, particularly for severe depression or suicidal ideation, where Spravato in particular is used, the immediate clinical goal is relief, and therapy can follow.
Some patients also reach a point where they don't want to be in therapy. That's a legitimate position. The treatments work without it.
What Elevium's Approach Looks Like in Practice
Elevium doesn't operate on a fixed template. Treatment plans are built around the individual, their diagnosis, history, goals, and preferences.
During your initial consultation, your clinician will assess which combination of treatments is likely to produce the best outcome for you. For some patients, that's TMS or ketamine as a primary intervention, with therapy introduced once neurological symptoms have stabilised. For others, starting both together from the beginning makes more sense.
What we don't do is push therapy on patients who don't want it, or assume that neuromodulation alone is always sufficient. The goal is an honest assessment of what's most likely to work for you, and a plan that reflects that.
Is therapy required to start TMS or ketamine at Elevium?
No. Both are available as standalone treatments. Therapy is recommended when it's clinically appropriate, not as a default requirement.
Can I add therapy partway through a TMS or ketamine course?
Yes, and for some patients this is actually the preferred sequence — stabilise neurological symptoms first, then introduce therapeutic work once you have the capacity to engage with it.
What type of therapy does Elevium offer?
We specialise in CBT and DBT, and also offer Interpersonal Therapy and Person-Centred Therapy. Your therapist will be matched to your specific goals and presentation.
What is ketamine-assisted psychotherapy?
It's an approach that integrates psychotherapy directly with the ketamine experience, using the neuroplasticity window to deepen therapeutic work. Elevium is developing this programme, ask your clinician for the latest on availability.
Share Article