Does Medicare Cover TMS, Spravato, or Ketamine?
If you're on Medicare and wondering whether your treatment is covered, the answer depends entirely on which treatment you're asking about. TMS and Spravato are both covered; ketamine infusions are not. Here's the full picture.
A Quick Note on How Medicare Works
Medicare is split into parts, and which part covers your treatment matters.
- Part A covers inpatient hospital care
- Part B covers outpatient services, doctor visits, procedures, and drugs that must be administered in a clinical setting
- Part C (Medicare Advantage) is a private plan that bundles Parts A and B, and must cover at a minimum everything Original Medicare covers
- Part D covers prescription drugs you take at home
TMS and Spravato both fall under Part B, because they require in-clinic administration and supervision, they're billed as outpatient medical services, not prescriptions. That distinction matters for how you're billed and what you'll pay.
If you have a Medigap (supplemental) policy, it may cover some or all of the 20% coinsurance that Part B leaves to you, which can significantly reduce your out-of-pocket costs for both treatments.
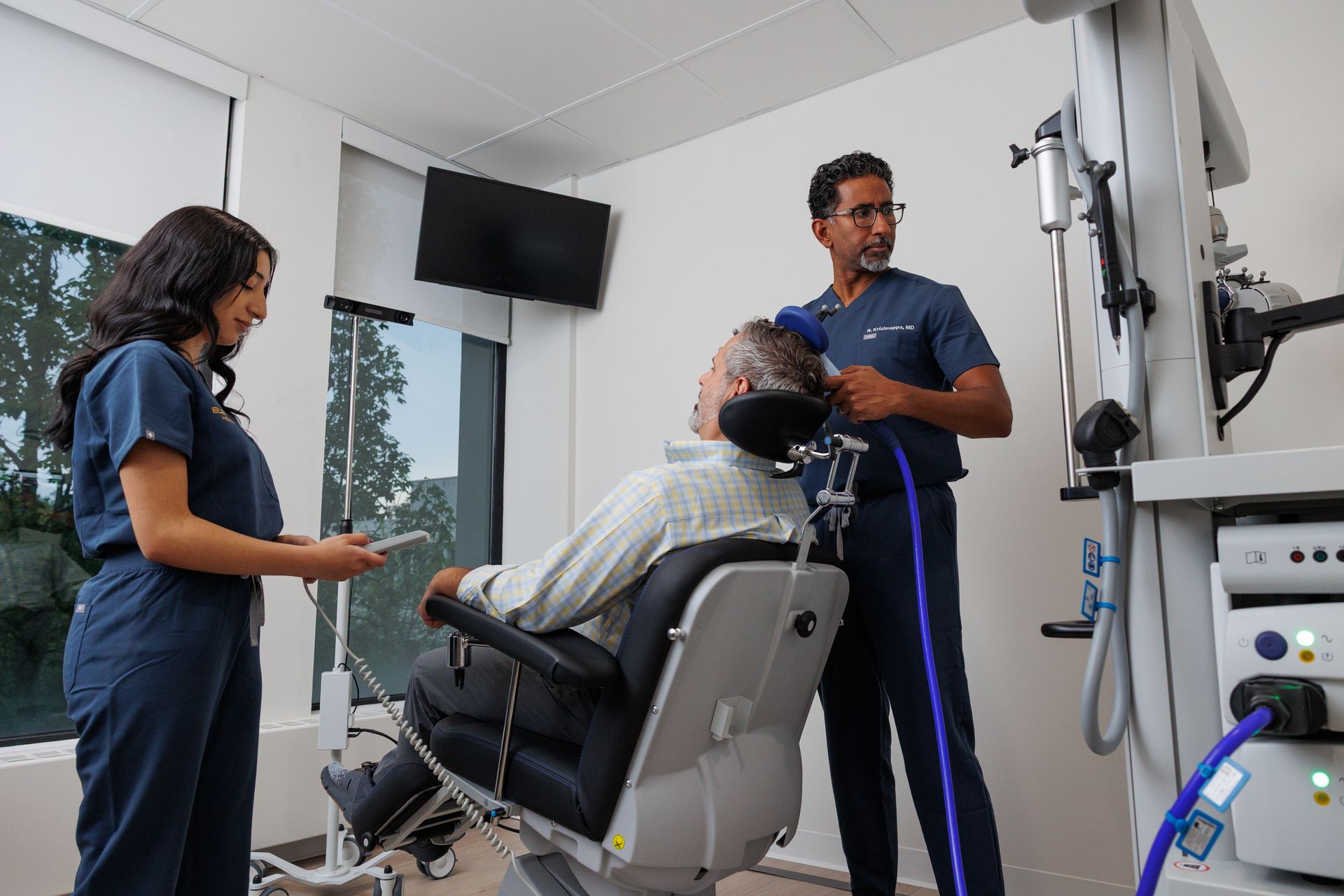
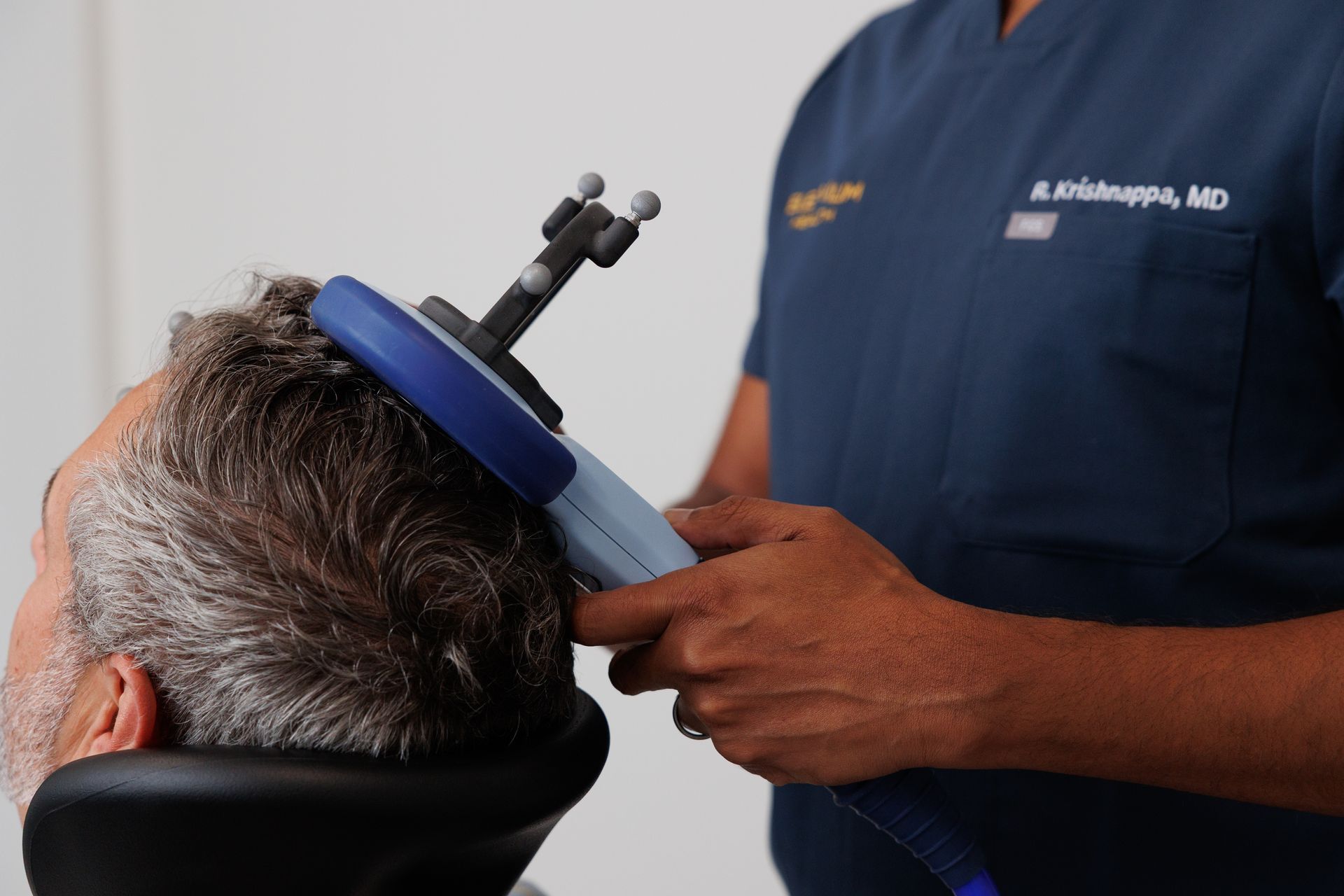
TMS and Medicare: Covered, With Conditions
Medicare Part B covers TMS for severe major depressive disorder. The keyword is severe, Medicare's coverage criteria are specific, and not everyone with depression will qualify automatically.
To be eligible, you generally need to:
- Have a confirmed diagnosis of severe MDD as defined by DSM-5 criteria
- Have tried at least one antidepressant that was either ineffective or intolerable
- Have a psychiatrist order the treatment following an in-person examination
Notably, Medicare's threshold is lower than most commercial insurers - one failed antidepressant trial (or documented intolerance) is generally enough, whereas private plans often require two to four.
What you'll pay: In 2026, Medicare Part B carries a $283 annual deductible. Once that's met, Medicare covers 80% of the approved amount for each session; you're responsible for the remaining 20% coinsurance. Medicare Advantage plans must cover at least what Original Medicare covers, though cost-sharing structures vary by plan. If you hold a Medigap (supplemental) policy, it may cover all or most of that 20%, bringing your out-of-pocket cost close to zero.
What Medicare won't cover for TMS: OCD, despite TMS being FDA-approved for OCD, Medicare's local coverage determinations have found insufficient evidence to support coverage for that indication.
TMS for anxiety, PTSD, or other conditions is also not covered. And certain contraindications, including magnetic implants within 30cm of the coil, or a history of seizures in some cases, will exclude you from coverage.
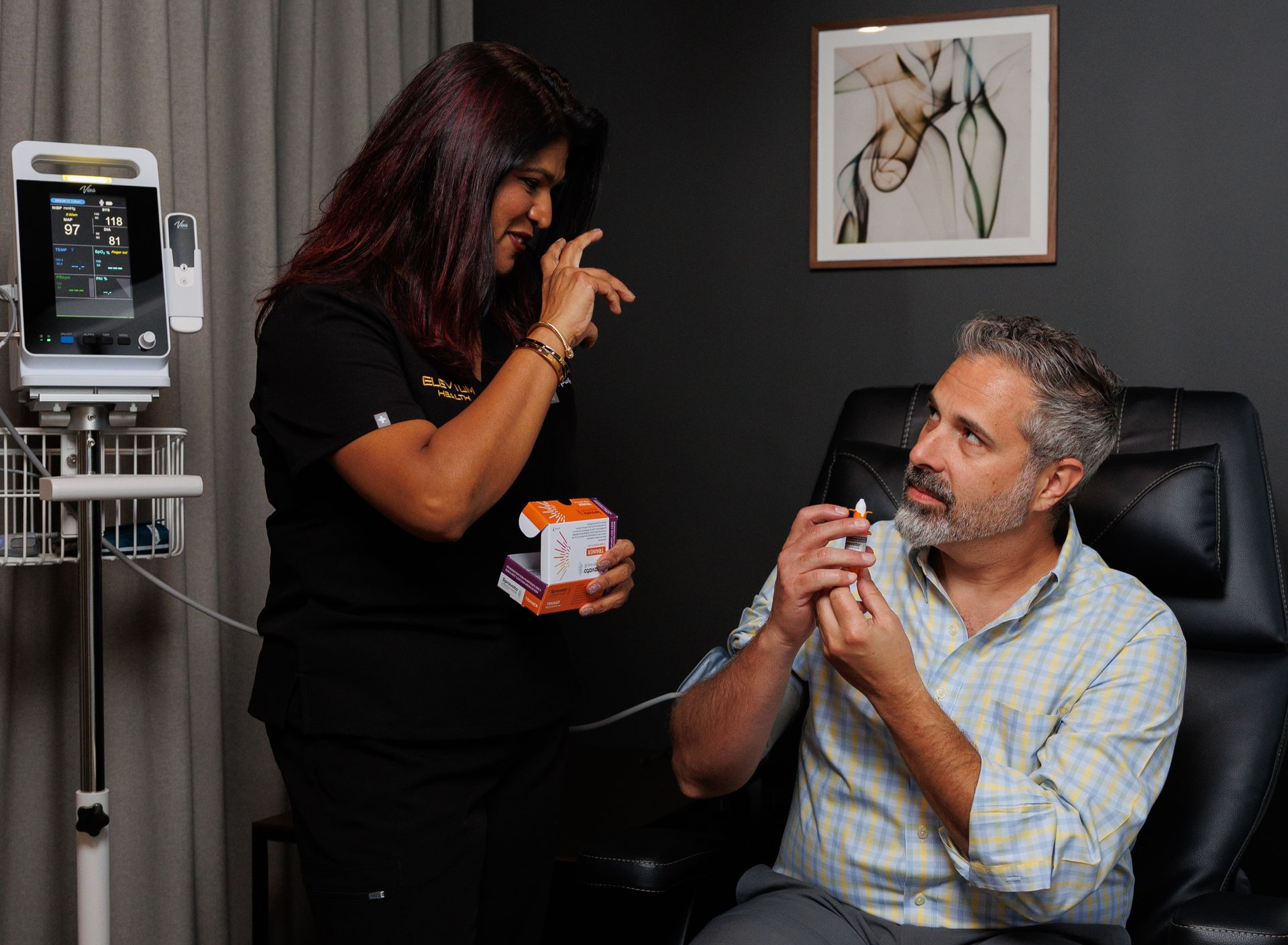
Spravato and Medicare: Covered as a Part B Drug
Spravato (esketamine) is covered under Medicare Part B (not Part D) because it has to be administered in a certified clinical setting rather than taken at home. Since every session requires on-site supervision and a two-hour monitoring period, it's billed as an outpatient medical service.
Elevium Health is a REMS-certified Spravato treatment centre, which is a requirement for Medicare billing.
To qualify, you need:
- A diagnosis of treatment-resistant depression (MDD that hasn't responded to at least two antidepressants)
- OR major depressive disorder with active suicidal ideation
- Documentation of those prior treatment attempts
What you'll pay: The same Part B structure applies, 80% covered by Medicare after the $283 deductible, with 20% coinsurance left to you. Spravato sessions involve both the drug cost and the monitoring service, and both are billed together. Per-session costs can be high, so the 20% coinsurance adds up during the induction phase (twice weekly for the first month). Medigap coverage, if you have it, can substantially reduce or eliminate that 20%. Medicare Advantage plans must cover Spravato, but typically require prior authorisation and may have different cost-sharing.
What Medicare won't cover: Spravato for any indication other than treatment-resistant depression or MDD with suicidal ideation. Documentation is required; Medicare won't cover it on clinical judgment alone.
Ketamine Infusions and Medicare: Not Covered
This is the straightforward one. Medicare does not cover IV, IM, or oral ketamine infusions for mental health treatment. The reason is regulatory, not clinical: ketamine is only FDA-approved as an anaesthetic. Its use for depression and other psychiatric conditions is off-label, and Medicare doesn't cover off-label psychiatric ketamine.
This doesn't mean ketamine therapy isn't effective; the evidence is strong, and it's widely used. It simply means you'll pay out of pocket for it at Elevium.
The exception worth knowing: if you're on a Medicare Advantage plan or hold supplemental private insurance, it's worth checking your specific policy. A small number of commercial plans have covered ketamine on a case-by-case basis, though it's uncommon. Submitting a superbill (an itemised receipt) to private insurers is an option some patients explore, though reimbursement is not guaranteed.
If cost is a barrier, Spravato is often the better-covered alternative with comparable outcomes for treatment-resistant depression.
How Elevium Handles Medicare Coverage
Elevium Health is a Spravato REMS-certified treatment centre in Florham Park, New Jersey, and we work with most major insurance plans, including Medicare and Medicare Advantage. Our team handles insurance verification — before you begin treatment, we'll check your specific benefits, confirm any prior authorisation requirements, and give you a clear picture of expected out-of-pocket costs.
The process is straightforward: book a consultation so your clinician can assess whether you're a clinical candidate, our team verifies your Medicare or Advantage benefits and submits any prior authorisation on your behalf, and treatment begins once authorisation is confirmed.
If you're a Medicare beneficiary in New Jersey considering TMS, Spravato, or another psychiatric treatment, contact Elevium Health to start a benefits check. There's no obligation, and you'll know where you stand before any decisions are made.
Does Medicare cover accelerated or one-day TMS?
Original Medicare coverage is for standard TMS protocols. Coverage for accelerated protocols varies; prior authorisation requirements and local coverage determinations may treat accelerated TMS differently. We'll verify this for your specific plan.
Can Medicare cover TMS and Spravato at the same time?
Potentially, yes, if you meet criteria for both. This would be assessed during your consultation based on your clinical presentation and treatment history.
What if my Medicare claim is denied?
Denials can be appealed. The most common reason for denial is insufficient documentation of prior treatment attempts. Elevium's team can help gather the records needed to support an appeal.
Does Medicaid cover these treatments in New Jersey?
Medicaid coverage varies by state and by treatment. Contact us directly and we'll run a benefits check for your specific Medicaid plan.
Share Article